HEALTH Committees recomendation supriya.pptx
- 1. HEALTH COMMITTEES Presenter: B Supriya Chhetry M.Sc. Nursing 2nd year
- 2. INTRODUCTION Health planning in India is an integral part of national socio-economic planning The guide-lines national health planning were Provided by a number of committees dating back to the Bhore committee in 1946 These committees were appointed by the Government of India from time to time to review the existing health situation and recommend measures for further action.
- 3. Committee This committee were appointed to review the existing health situation and recommend measures for further action. The goal of National Health Planning in India was to attain Health for all by the year 2000 by the Alma-Ata declaration on primary health care.
- 5. BHORE COMMITTEE, 1946 • Chairman: Sir. Joseph Bhore, an Indian Civil servant. • Setup in 1943 • Also known as ‘Health Survey and Development committee’. • During pre-independence era, to improve the Comprehensive health care (preventive, promotive and curative) health services of country, a National Planning Commission was set up by the Indian National Congress in 1938. The rulers of that time, the British Empire realised the importance of Public Health and instituted the ‘Health Survey and Development Committee,’ in the year 1943.
- 6. BHORE COMMITTEE, 1946 The committee was conducted the survey the about health conditions and health organisations in the country, and to make recommendations for future development. The committee submitted its report in1946. The integration of preventive, promotive and curative health services and establishment of Primary Health Centres in rural areas were the major recommendations made by this committee. School health. 3 Months training in preventive and social medicine to prepare social physicians.
- 7. OBSERVATION BY COMMITTEE: • “If the nation’s health is to be build, the health programme should be developed on a foundation of preventive health work and that such activities should proceed side by side with those concerned with the treatment of the patients.” • Committee dealing with the subjects :- o Medical relief o Medical research o Industrial health o Professional educations o Public health
- 8. OBSERVATIONS MADE BY THE COMMITTEE. 1.Health status of the country as indicated by various indicators was poor. 2.Mortality rates were very high. 3.Life expectancy at birth was about 27yrs. 4.Incidence of communicable diseases was very high. 5.Many of the health problems were preventable. 6.Committee stated that health and development are interdependent. 7.Improvement in sector other than health will also lead to improvement in health like water supply, sanitation improvement, nutrition ,elimination of unemployment.
- 9. GUIDING PRINCIPLES ADOPTED No individual should be denied to secure adequate medical care because of inability to pay. Facilities for proper diagnosis and treatment. Health programme must lay special emphasis on preventive work. As much medical relief and preventive health care should be provided to the vast rural population. Health services should be located close to the people to ensure maximum benefit to the community. Doctor should be a social physician protecting the people. Medical services should be free to all, without distinction.
- 10. PURPOSE 1.To survey the existing Health conditions and Health organization and to give suggestions for future development. 2.Primarily to review those activities within the scope of health administration.
- 11. BHORE COMMITTEE SUBMITTED ITS REPORT IN 1946 First time proposed a national program for improving health services in the country. The committee observed: “if the nation’s health is to be built, -the health program should be developed. 1.On a foundation of Preventive health. 2.Preventive activities should proceed side by side with those concerned with the treatment of patients.
- 12. BHORE COMMITTEE SUBMITTED ITS REPORT IN 1946 • The report consisted 4 volumes: Volume I - A survey of the State of the Public Health and the existing health organisation. Volume II Recommendations. Volume III Appendices. Volume IV Summary.
- 13. SOME IMPORTANT RECOMMENDATIONS BY BHORE COMMITTEE 1. Integration of preventive and curative services at all administrative levels. • Minimum required ratio 567 hospital beds,62 doctors,151 nurses per 1,00,000 population. 2. Development of primary health centres in 2 stages: A) Short term measures B) Long term measures 3. Major changes in medical education which includes 3 - month training in preventive and social medicine to prepare “social physicians”
- 14. SHORT TERM MEASURES A progressive improvement of public health depends largely on the promotion of the hygienic mode of life among the people The bed-population ratio should be raised from 0.24 per 1,000 to 1.03 at the end of 10 years Personal and impersonal health services should be provided. Dental sections should be established in the hospitals at secondary health center. Provision of housing accommodation for health staff is essential in the interests of efficiency.
- 15. CONT. Village communications should be developed in order to enable health organizations to provide efficient service For each 30-bed hospital, there should be two motor ambulances and one animal-drawn ambulance. Traveling dispensaries should be provided to supplement the health services rendered by primary health center in sparsely populated areas.
- 16. LONG TERM MEASURES Public health personnel: Nutrition: Health education: Physical education: School health services: Occupatio nal health including industrial health: Environm ental hygiene:
- 17. DEVELOPMENT OF PRIMARY HEALTH CENTRES IN 2 STAGES: • 1. Primary health centre in the rural areas 1/40,000 population 2. Secondary health centre to serve as a supervisory, coordinating and referral institution. • The short term 1 PHC should cater to a population of 40,000, 30 beds, 3 subcentres. Staff suggested for each PHC, – 2medical officers, – 4 public health nurses, – 1nurse, – 4 midwives, – 4 trained dais, – 2 sanitary inspectors, – 2 health assistants, – 1pharmacist, and – 15 other class IV employees were recommended. SHORT TERM MEASURES
- 18. CONT.. • This primary unit would have adequate ambulatory support to link it to the secondary unit when the need arises for secondary level care. • Each province was given the autonomy to organize its primary units in the way it deemed most suitable for its population, but there was to be no compromise on quality and accessibility.
- 19. DEVELOPMENT OF PRIMARY HEALTH CENTRES IN 2 STAGES: To setup primary units with 75 bedded hospitals for each 10to20 thousand population and secondary unit with 650 bedded hospital, again regionalized around district hospital with 2500 beds. It was proposed to have major changes in medical education which includes:- “3 months training in preventive and social medicine to prepare social physicians”. Primary Unit – PHC, First Tier Secondary Unit- CHC, Second Tier District Hospital, Third Tier LONG TERM PROGRAMME {Termed as “3 million plan”}
- 20. PRIMARY UNIT: PRIMARY HEALTH CENTRE Every 10,000 to 20,000 population (depending on density from one area to another) • would have a 75-bedded hospital. Served by Six Medical Officers including medical, surgical and obstetrical and gynaecological specialists. This medical staff would be supported by 6 public health nurses, 2 sanitary inspectors, 2 health assistants and 6 midwives to provide domiciliary treatment. At the hospital there would be a complement of 20 nurses, 3 hospital social workers, 8 ward attendants, 3 compounders and other non-medical workers.
- 21. PRIMARY UNIT: PRIMARY HEALTH CENTRE • The Two medical officers along with the public health nurses would engage in providing preventive health services and curative treatment at homes of patients. • The sanitary inspectors and health assistants would aid the medical team in preventive and promotive work. Preferably at least three of the six doctors should be women. The 75 beds, 25 would cater to medical problems, 10 for surgical, 10 for gynaecological, 20 for infectious diseases, 6 for malaria and four for tuberculosis.
- 22. SECONDARY UNIT Click icon to add pictur First level referral hospital. The secondary unit would be a 650-bedded hospital having all the major specialities with: a staff of 140 doctors, 180 nurses and, 178 other staff including 15 hospital Social Workers, 50 ward attendants and 25 compounders. The secondary unit besides being a first level referral hospital would supervise, both the preventive and curative work of the primary units.
- 23. CONT.. • Note:The 650 beds of the secondary unit hospital would be distributed as follows: Medical 150, Surgical 200, Obs. & Gynae 100, Infectious Disease 20, Malaria 10, Tuberculosis 120, and Paediatrics 50.Total 650.
- 24. DISTRICT HOSPITAL Every district centre would have a 2500 beds hospital providing largely tertiary care with 269 doctors, 625 nurses, 50 Hospital Social Workers and 723 other workers. The hospital would have 300 medical beds, 350 surgical beds, 300 obs. & gynae beds, 540 tuberculosis beds, 250 paediatric beds, 300 leprosy beds, 40 infectious diseases beds, 20 malaria beds and 400 beds for mental diseases.
- 25. CONT.. • A large number of these district hospitals would have medical colleges attached to them. However, each of the three levels would have functions related to medical education and training, including internship and refresher courses.
- 26. RECOMMENDATIONS 3 months training in preventive and social medicine to prepare ‘SOCIAL PHYSICIANS’ Special emphasis on preventive work (Integration of curative and preventive services) Village Health Committee consisting of 5 to 7 individuals for procuring the active participation of the people in the local health programme.
- 27. CONT.. • Inter-sectoral Coordination. • This document laid the utmost emphasis on primary health care; it needs no emphasis that primary health care was later on recognised as the key strategy to achieve Health for All (HFA) by 2000 during Alma-Ata conference. • The Bhore committee model was based on the allopathic system of medicine.The traditional health practices and indigenous system of medicine prevalent in rural India, which had great influence and were part of their socio-cultural milieu were not included in the model proposed by Bhore committee
- 28. POST INDEPENDENCE ERA: With the beginning of health planning in India and first five-year plan formulation (1951- 55), Community Development Programme was launched in 1952 for the all round development of rural areas, where 80% of the population lived. Community Development was defined as "a process designed to create conditions of economic and social progress for the whole community with its active participation and the fullest possible reliance upon the community's initiative". The Community Development Programme was envisaged as a multipurpose programme covering health and sanitation (through the establishment of primary health centres and sub-centres) and other related sectors including agriculture, education, transport, social welfare and industries. Each Community Development Block (CDB) comprised approximately 100 villages with a total population of one lakh. For one CDB, one Primary Health Centre was created.
- 29. MUDALIAR COMMITTEE, 1962 The Mudaliar committee, popularly known as the “Health Survey and Planning Committee.” Mudaliar Commission is an education commission set up with the aim of examining the system of secondary education in India. It is also called as Secondary Education Commission which has been come in 1952- 1953. Chairman: Dr. A Laxman Swami Mudaliar.
- 30. MUDALIAR COMMISSION INTRODUCTION • The Secondary Education commission known as Mudaliar Commission was appointed by the government of India in term of their Resolution to bring changes in the present education system and make it better for the Nation. Dr. A. Lakshmanswami Mudaliar was the Vice-Chancellor of Madras University. • After the Independence India needed a change in the education system. Number of Secondary Schools were increasing in India it was much a need to take care the students of secondary school.
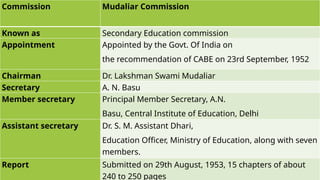
- 31. Commission Mudaliar Commission Known as Secondary Education commission Appointment Appointed by the Govt. Of India on the recommendation of CABE on 23rd September, 1952 Chairman Dr. Lakshman Swami Mudaliar Secretary A. N. Basu Member secretary Principal Member Secretary, A.N. Basu, Central Institute of Education, Delhi Assistant secretary Dr. S. M. Assistant Dhari, Education Officer, Ministry of Education, along with seven members. Report Submitted on 29th August, 1953, 15 chapters of about 240 to 250 pages
- 32. The system of successive 5-year plans – For organized development of the country –Started in 1951. As the Second Five Year Plan (1956-61) was ending – >10 yrs. had elapsed following Bhore committee report. Guidelines for further development of National health services were needed – In the context of the Five year Plans. In 1959, the Government of India appointed another Committee known as – "Health Survey and Planning Committee", – Popularly known as the Mudaliar Committee 1. To survey the progress made in the field of health – Since submission of the Bhore Committee's Report (1946) 2. To make recommendations for future development and expansion of health services. The committee submitted its report in 1962
- 33. THE MUDALIAR COMMITTEE FOUND: • Quality of healthcare provided by the primary health centres was unsatisfactory. Felt the need for strengthening the: 1. Existing primary health centres – Before new centres were established. 2. Sub-divisional and district hospitals – so that they may effectively function as referral centres.
- 34. THE COMMITTEE WAS SUB-DIVIDED INTO DIFFERENT SUB-COMMITTEES TO DEAL WITH DIFFERENT SUBJECTS: 1.Medical Care 1.Public Health 1.Control of communicabl e disease 1.Population control 1.Profession and research
- 35. THE COMMITTEE WAS SUB-DIVIDED INTO DIFFERENT SUB-COMMITTEES TO DEAL WITH DIFFERENT SUBJECTS: 1.Indigenous system of medicine 1.Drugs and medical supplies 1.Legislation 1.Health administratio n 1.Medical research
- 36. MAIN RECOMMENDATIONS OF THE MUDALIAR COMMITTEE, 1962 • (1) Consolidate the progress made in first 2 five-year plans. (2) Strengthen the district hospitals with Specialists – So that they can act as good referral centers and – To serve as central base of regional services (3) Create a regional administrative level in between the headquarters at state level and the district level. – In charge of a Regional Deputy or Assistant Directors – Each to supervise 2 or 3 district medical and health officers.
- 37. MAIN RECOMMENDATIONS OF THE MUDALIAR COMMITTEE, 1962 (4) Each primary health centre should cater to a maximum of 40,000 population. (5) To improve the quality of health care provided by the primary health centres. (6) Integration of medical and health services as recommended by the Bhore Committee. (7) Constitution of an ‘All India Health Service’ on the pattern of ‘Indian Administrative Service’ (IAS).
- 38. RECOMMENDATIONS RELATED TO NURSING SECTORS ARE AS FOLLOWS There should be 3 grades of nurse viz the basic nurses (with 4 year training)the auxiliary nurse wife (2 year training )and the nurse with a degree qualification The medium of instruction should preferably be English for the general nursing course, while the degree course should be taught only in English. In view of the need for securing a larger number of recruits for the nursing profession the age of at mission can be reduced to 16 in suitable cases as a transitional measure particularly in states where there are difficulties in recruiting candidates at the age of 17. . Candidates admitted to the general nursing course should have the minimum qualification of matriculation or equivalent and the candidates degree course should have passed the higher secondary or preuniversity examination
- 39. CONT.. 5. Nurse pupils should not be overburdened with the routine duties in hospitals, but more attention should be given to training and practical experience.They should not be subjected to too many spells of night duties in hospitals. 6.To train more nurses a large number of hospitals in the country could be utilized for nursing schools. District headquarters hospitals with a bed strength of 75-100 should also be utilized for this purpose. 7. Student nurses should be provided free furnished accommodation in hospitals, free board, free supply of uniforms, laundry arrangements, free books, free medical services, medical checkup twice a year and suitable recreational facilities.The stipend during training should be a minimum of 35 ₹ increasing by *10 every year. 8.The minimum of admission to the course should be 12.
- 40. CONT.. 9. The recommendations of the committee set up by the Central Council of Health (Shetty committee) in regard to pay scales and ratio of nurses to hospital beds, etc. are enclosed. 10.There should be a nursing advisory committee in each school for advising on admission and welfare of the trainees. 11. Each nursing school should have its own separate budget. 12.The training of auxiliary nurse midwives should be continued and extended, because it will be necessary for a long time to come to have a second line of trained personnel to meet the needs of the country.
- 41. CONT.. 13.The number of auxiliary nurse midwives to be trained should be phased in such a way that there will be one auxiliary nurse midwife for 5,000 population by the end of 15 years. 14.The training of midwives should also be continued and they should replace the dais, who is now being utilized at certain places. 15.The time is come when fresh thinking on the type of training at present given to health visitors should be done.There should, instead, be public health nurse with a basic nursing qualification and 1 year's further training particularly in domiciliary care and other public health aspects of community work. 16.The continuance of the training of dais in certain states as a temporary measure is recommended, till such time a sufficient number of midwives are trained to replace them
- 42. CONT.. 17.Any person trained in one category of nursing should get an opportunity of being trained in the next higher grade, under conditions to be specified by the Indian nursing council. 18.There should also be higher training for the general sick nurse, public health nurse, pediatric nurse, mental diseases nurse, theater sister, tutor and nursing administrator. 19. Promotion of degree course nurses and of basic nurses to posts of higher responsibility should be considered only after a minimum of 3- 5 years of practical experience after qualification has been obtained.
- 43. CHADHA COMMITTEE, 1963 Also known as “special committee on the preparation of entry of National Malaria Eradication Program into Maintenance Phase”. Appointed by the Government of India in 1963 – Under the Chairmanship of Dr. M.S. Chadah. – The then Director General of health Services To study the arrangements necessary for – the maintenance phase of the National Malaria Eradication Programme (NMEP).
- 44. WHY THE CHADHA COMMITTEE? • • Malaria used to be rampant in India in 1950’s – It was the greatest handicap in the socio-economic development of the country • National Malaria Control Program (later NMCP) was launched in 1953 – to control the extremely high levels of Malaria infections
- 45. PURPOSE OF CHADHA COMMITTEE: •Study the requirement related to: a)PHCs planning & priority according to needs of Maintenance Phase of NMEP. b)Staffing pattern for NMEP and how to utilise NMEP staff post eradication status.
- 46. KEY OBSERVATIONS: Wide variations in malaria situation & control. Re-emergence likely unless eradicated globally.
- 47. THE COMMITTEE CONSIDERATE TO:- a. The absorption of the activities of the maintenance phase into the general health services. b.Strengthening of basis rural health services. c. Training of personnel engaged in specialized mass campaigns to become multipurpose workers to that they can continue to follow-up the measures required for the maintenance phase as a part of the routine health activities.
- 48. THE PROGRAM OPERATED IN 4 PHASES • 1. Preparatory 2. Attack 3. Consolidation 4. Maintenance: House to house visits to identify fever cases (Vigilance) • • A special organization was established for the first 3 phases • The ‘Maintenance’ phase: the responsibility for the activities was to be passed on to the General health services of the country in 1964 • • Chadha committee was appointed – To identify the arrangements for this important hand over of the maintenance phase.
- 49. THE COMMITTEE RECOMMENDED: • • ‘Vigilance’ operations under NMEP. – Should be the responsibility of the general health services i.e. – Primary health centres at the block level. • Vigilance operations included: – Monthly home visits to identify fever cases – To be carry out through separate workers
- 50. THE COMMITTEE RECOMMENDED: • • The ‘basic health workers’. – One basic health worker per 10,000 population was recommended. • The Basic health workers were seen as ‘multipurpose workers’ i.e. 1. In addition to malaria vigilance, have duties of 2.Collection of vital statistics and 3.Family planning • The Family Planning Health Assistants were – To supervise 3 or 4 of these basic health workers. • • From the district level upwards: – The general health services were to take the responsibility for the maintenance phase.
- 51. MUKERJEE COMMITTEE, 1965 Also known as ‘to review strategy of family planning’ Appointed on 31st December, 1965. Under the Chairmanship of Shri B. Mukherji the then Secretary, Ministry of Health and Family Planning, government of India, was appointed to review the strategy for the family planning programme. In a short time after implementation of Multiple Health Worker (MPHW) scheme it was realised that malaria vigilance operations & family planning program could not be carried out effectively.
- 52. MUKERJEE COMMITTEE, 1965 A committee known as Mukerjee committee was formed in 1965 & it recommended separate staff for Family planning activities so that malaria activities could receive undivided attention of its staff. In 1966 Basic health services should be provided at the block level.
- 53. PURPOSE OF MUKERJI COMMITTEE • To review what changes are necessary in staffing pattern, financial provisions, etc. due to IUCD gaining prominence in the Family Planning Programme.
- 54. KEY OBSERVATIONS OF MUKERJI COMMITTEE • Great shortage of staff for Family Planning (FP) Programme Doctors are reluctant to take up Family Plannings duties Training, infrastructure lacking/deficient.
- 55. THE COMMITTEE RECOMMENDED: Strengthening of state health department by providing additional staff sanctioned by central government. There should be a separate cell in the state sectorial for by under secretarial/assistant secretary with a small supporting staff, which are:- • -Under secretariat/assistance Secretary-1 • -U.D. assistant-1 • -Stenotypical-1 • -Orderly person-1 Creation of post of lady health visitor (LHV)
- 56. THE COMMITTEE RECOMMENDED: There should be one family planning field worker (FPFW) for every 2 subcenters Part-time workers for motivating population for acceptance of IUD (intrauterine device). Block and district level education leaders be appointed for intensifying motivation campaign and be paid honorarium of rupee 600/- per annum. Government dr. may be provided incentives which should also be available to part-time private medical practitioners in terms of honorarium of rupee 100.
- 58. JUNGALWALA COMMITTEE, 1967 This committee is also known as “Committee on Integration of Health Services”. Appointed on 1964. Chairperson: Dr. Nowshir Jungalwalla.
- 59. AIMS:- To integrate the health services and elimination of private practice by government doctors.
- 60. PURPOSE OF JUNGALWALA COMMITTEE: To examine various problems including service conditions; elimination of private practice.
- 61. KEY OBSERVATION: •Non-practice allowance should be reasonable and realistic to prevent private practice.
- 62. RECOMMENDATION OF THIS COMMITTEE: 1.Equal pay for equal work 2.Abolition of private practices by govt. doctors. 3.Recognition of extra qualification 4.Common seniority 5.Special pay for specialized work. 6.Improvement in their service conditions 7.Unified cadre.
- 63. KARTAR COMMITTEE, 1973 This committee is also known as “The Committee on Multipurpose Workers (MPW) under the Health and Family Planning Programme”. Appointed on 28 October 1972. Chairperson: Mr. Kartar Singh
- 64. PURPOSE OF KARTAR COMMITTEE: • To study & make recommendations on: The structure for integrated services at the peripheral & supervisory levels. The feasibility of having multipurpose, bi-purpose workers in the field The training req. for such workers The utilization of mobile service units under FP programme for integrated national, public health & FP services operating from taluk level.
- 65. KEY OBSERVATION: Generally, 1 PHC/80k-110k or more . There are wide disparities in staffing; wide variation in pay scales between states Community leaders unhappy with many workers visiting homes under individual programmes, prefer single visit FP, malaria, smallpox workers feel ability to provide treatment for minor ailments during field visits will increase acceptability in community. Poor performance of peripheral workers largely due to inadequate supervision.
- 66. MAJOR RECOMMENDATION: Having multipurpose workers is desirable & feasible Integrate vertical programmes at all levels Create new job description and designations: ANM Health Worker (Female) → Male MPW Health Worker (Male) → Supervisors Health Supervisor (Male/Female) → 1 Health Supervisor/ 4 Health Workers 1 PHC/6 Sub-centres (3100 pop each) [1PHC/50k pop.]
- 67. •Impact: Many vertical progs. suffered as MPWs were unable to do work previously done by dedicated staff. Resurgence of malaria. Resentment from dedicated staff as they were used for general health activities.
- 68. SHRIVASTAVA COMMITTEE, 1975 • The issue of developing alternative strategy for the delivery of health services and rationalisation of the health manpower both in terms of number of personnel as well as categories of personnel had been engaging the attention of the Govt. of India from time to time. • The Govt. of India in the Ministry of Health and Family Planning had in November 1974 set-up a "Group on Medical Education and Support Manpower" • under the chairmanship of Dr JB Shrivastav, then the DGHS was established to focus on this issue.
- 69. • The terms of reference of this committee were as follows: 1.To devise a suitable curriculum for training a cadre of health assistant conversant with basic medical aid preventive and nutritional services, family welfare, maternity and child welfare activities so that they can serve as link between the qualified medical practitioners and the multipurpose workers, thus forming an effective team to deliver health care, family welfare and nutritional services to the people.
- 70. • The terms of reference of this committee were as follows: 1.Keeping in view the recommendations made by the earlier committees on Medical Education, specially the Medical Education Committee (1968) and the Medical Education conference (1970), to suggest suitable ways and means for implementation of these recommendations, and to suggest steps for improving the existing medical educational processes so as to provide due emphasis on the problems particularly relevant to national requirements, and 2.To make any other suggestions to realise the above objectives and matters incidental thereto.
- 71. RECOMMENDATIONS BY THE COMMITTEE • After carefully examining various reports and papers relevant to the subject including the recommendations of as many as 12 conferences and committees, held earlier, Shrivastav Group, made following major recommendations: 1. A nationwide network of efficient and effective services suitable for our conditions, limitations and potentialities should be evolved 2. Steps should be taken to create bands of paraprofessionals or semi-professional health workers from the community itself to provide simple, protective, preventive and curative services which are needed by the community. 3. Between the community and the primary health center, there should be two cadres, health workers and health assistants. - Health workers should be trained and equipped to give simple, specified remedies for day- to-day illness.
- 72. RECOMMENDATIONS BY THE COMMITTEE - Health assistants would work as intermediaries between the health workers and primary health centres. They also should be trained and equipped to give simple specified remedies for simple illnesses according to their level of technical competence. The primary health center should be provided with an additional doctor and nurse to look after the maternal and child health services. The possibility of utilizing the services of senior doctors at the Medical college, regional, district/ taluk hospitals for brief periods at PHC should be explored.
- 73. • Acceptance of the recommendations of the Shrivastava Committee in 1977 led to the launching of the Rural Health Service.
- 74. RESEARCH STUDY 1. Using Community-based Evidence For Decentralized Health Planning: Insights from Maharashtra, India • Abhay Shukla,1* Renu Khanna2 and Nitin Jadhav1 1.Support for Advocacy and Training to Health Initiatives (SATHI), 3&4 Aman Terrace-E, Dahanukar Colony, Kothrud, Pune 411029, India, 2.AHAJ - Society for Health Alternatives, Vadodara-390007, Gujarat, India.Accepted 29 July 2014 • Health planning is generally considered a technical subject, primarily the domain of health officials with minimal involvement of community representatives.The National Rural Health Mission launched in India in 2005 recognized this gap and mandated mechanisms for decentralized health planning. However, since planning develops in the context of highly unequal power relations, formal spaces for participation are necessary but not sufficient. Hence a project on capacity building for decentralized health planning was implemented in selected districts of Maharashtra, India during 2010–13. • This process developed on the platform of officially supported community-based monitoring and planning, a process for community feedback and participation towards health system change. A specific project on capacity building for decentralized planning included a structured learning course and workshops for major stakeholders.
- 75. CONTD • •An evaluation of the project, including in-depth interviews of various participants and analysis of change in local health planning processes, revealed positive changes in intervention areas, including increased capacity of key stakeholders leading to preparation of evidence-based, innovative planning proposals, significant community-oriented changes in utilization of health facility funds, and inclusion of community-based proposals in village, health facility-based block and district plans.Transparency related to planning increased along with responsiveness of health providers to community suggestions. • •A key lesson is that active facilitation of decentralized health planning and influencing the health system to expand participation, are essential to ensure changes in planning. Effective strategies included: identifying people’s health service-related priorities through community-based monitoring, capacity building of diverse stakeholders regarding local health planning, and advocacy to enable participation of community-based actors in the planning process.This combination of strategies draws upon the framework of ‘empowered participatory governance ‘which necessitates combining a degree of ‘countervailing power’ and acceptance of participation by the system, for new forms of governance to emerge
- 76. Health and Human Rights Journal 2. Using Health Committees to Promote Community Participation as a Social Determinant of the Right to Health: Lessons from Uganda and South Africa • Moses mulumba, leslie london, juliana nantaba, and charles ngwena • Abstract • Community participation is not only a human right in itself but an essential underlying determinant for serves them efficiently. As acknowledged by the Rio Political Declaration on Social Determinants of Health, participatory processes are important in policy making and in the implementation of laws relating to health. Collective deliberation improves both community development and health system governance, resulting in more reasoned, informed, and public-orienteddecisions.1 More recently, attention has focused on the elements of health system governance that enable greater responsiveness to community needs. However, there is relatively little by way of interventions linking human rights approaches to governance in ways that recognize participation as a critical social determinant of the right to health.This paper provides perspectives from a three-year intervention whose general objective was to develop and test models of good practice for health committees in South Africa and Uganda. It describes the aspects that we found critical for enhancing the potential of such ommittees in driving community participation as a social determinant of the right to health.
- 78. QUIZ QUESTION • Which committee is known as health survey and developmental committee? 1. Bhore Committee 2.Chadha Committee 3. Mukerji Committee 4. Jungalwalla Committee 5. Kartar Singh Committee Right Answer is : 1. Bhore Committee
- 79. • Three tier system of health care delivery in rural area based on the recommendations of • A. Bhore committee • B. Mudalir committee • C. Srivastav committee • D. Kartar Singh Committee • Right Answer is : • ✓ C. Srivastav committee
- 80. • Chairman of health survey and planning committee was • A. Sir Joseph Bhore • B. Dr. A.L. Mudaliar • C. Kartar Singh • D. Srivastav • Right Answer is : • ✓ B. Dr. A.L. Mudaliar
- 81. •What was the goal of National Health Planning? •The goal of National Health Planning in India is to attain Health for all by the year 2000
- 82. • What does NITI Aayog stand for? 1.National Institute for Technology India 2.National Institute for Transforming India 3.National Interest for Technology India 4.National Interest for Transforming India
- 83. Which was the last 5 year planned and when did it ended? Ans :Twelfth Five-Year Plan (2012-2017)
- 84. REFERNCE: Government of India, Health Survey and Development (Bhore) Committee, Report, Volume-1, Delhi, Publications Division, 1946 National Planning Committee, Subcommittee on National Health (Sokhey) Committee, Report, Bombay, Vora, 1948 World Health Organization, Primary Health Care. Report of International Conference on Primary Health Care, Alma Ata, USSR, September 6-12, 1978, Geneva, WHO, 1978. Government of India. National Health Policy 2002, New Delhi, Ministry of Health and Family Welfare, 2002. Government of India, National Rural Health Mission: Mission Document, New Delhi, MOHFW, 2005 Indian Public Health Standards (IPHS) for Community Health Centers, Draft Guidelines, Directorate General of Health Services, MOHFW, GOI, April 2005 http://www.nihfw.org/reportsofncc.aspx https://gmch.gov.in/estudy/e%20lectures/Community%20Medicine/Health%20Plann https://www.nhp.gov.in/miscellaneous/committees-and-commissions • Mulumba, M., London, L., Nantaba, J., & Ngwena, C. (2018). Using Health Committees to Promote Community Participation as a Social Determinant of the Right to Health: Lessons from Uganda and South Africa. Health and human rights, 20(2), 11–17.
































































![MAJOR RECOMMENDATION:
Having multipurpose workers is desirable & feasible
Integrate vertical programmes at all levels
Create new job description and designations:
ANM Health Worker (Female)
→
Male MPW Health Worker (Male)
→
Supervisors Health Supervisor (Male/Female)
→
1 Health Supervisor/ 4 Health Workers
1 PHC/6 Sub-centres (3100 pop each) [1PHC/50k pop.]](https://image.slidesharecdn.com/healthcommitteesrecomendationsupriya-241220080010-8079f364/85/HEALTH-Committees-recomendation-supriya-pptx-66-320.jpg)



















