ACUTE PANCREATITIS combined.pptx.pptx in kids
- 1. PANCREATITIS Presenter : Dr. Vikas Sharma Moderator : Dr. Raghvendra Singh
- 2. Case Scenerio • 7 years/ male presented to a private hospital on 31st July 2019 with c/o pain in upper abdomen for 1 day, moderate to severe intensity, associated with nausea and vomiting Past history – non-significant Family history – GB calculi in mother • Examination – Conscious, oriented, vitals – stable P/A – soft, non-distended, epigastric tenderness+
- 3. • Inv – Serum amylase – 632 (normal range 20-80) Serum lipase – 1935 (normal range 0-160) CECT abd – Pancreas diffusely bulky and edematous with heterogenous contrast enhancement, mild peripancreatic fat stranding, mild- moderate free fluid in abdomen and pelvis
- 4. • SCOPE OF THE SEMINAR • Pancreas - Anatomy and Development - Physiology - Definition - Epidemiology - Classification - Pathophysiology - Etiology - Clinical features - Diagnosis - Management - Complications - Prognosis - Pancreatic enzymatic replacement in chronic pancreatitis
- 5. ANATOMY OF PANCREAS • The pancreas lies mostly posterior to the stomach • Retroperitoneal structure except for a small part of its tail • Consists of head, uncinate process, neck, body and tail • Head and neck overlies vertebrae
- 6. The main pancreatic duct + Common bile duct Hepatopancreatic ampulla (Ampulla of Vater) Opens at major duodenal papilla (2nd part of duodenum) • The accessory pancreatic duct opens at minor duodenal papilla Accessory pancreatic duct Main pancreatic duct
- 7. DEVELOPMENT • Dorsal pancreatic bud - invades dorsal mesentery. • Ventral pancreatic bud (uncinate process and inferior part of head) - develops from the duodenal wall close to the bile duct. • With the rotation of stomach and the duodenum, ventral pancreatic bud moves posterior and inferior to the dorsal pancreatic bud to fuse with it. • Ventral pancreatic bud forms main pancreatic duct (of Wirsung), which opens to major duodenal papilla.
- 8. DEVELOPMENTAL ABNORMALITIES • Pancreas divisum – 10% individuals, dorsal and ventral bud duct fail to fuse minor papilla draining the body and tail risk of recurrent pancreatitis. Diagnosis – ERCP, MRCP • Anomalous pancreaticobiliary union (APBU) – common bile duct and the main pancreatic duct unite outside duodenal wall channel more than 15mm in length increased risk of recurrent pancreatitis and cholangiocarcinoma. Pancreas divisum
- 9. • Annular pancreas – The ventral bud becomes misaligned encircling the second part of duodenum. Presentations – Neonatal bowel obstruction, can be associated with GIT malformations, chronic pancreatitis (rare) P
- 10. PHYSIOLOGY • More than 80% of the exocrine pancreas composed of clusters of acini lobules. • The basolateral membrane of the acini cells - receptors for cholecystokinin (CCK), acetylcholine, vasoactive intestinal peptide (VIP). • The acini cells - digestive enzymes • The centro-acinar cells and the duct cells - water and bicarbonate.
- 11. PANCREATIC SECRETIONS Pancreatic enzymatic pathways – 1) Proteolytic (a) Trypsin – cleaves interior peptide bonds involving basic amino acids. (b) Carboxypeptidase – cleaves at carboxy terminals (c) Chymotrypsin – cleaves interior bonds involving aromatic amino acids, leucine, glutamine and methionine (d) Elastase – cleaves at neutral aliphatic amino acids. (Pediatric Gastrointestinal and Liver Disease, Wyllie and Hyams, 3rd edition)
- 12. 2) Pancreatic triglyceride lipase (PTL) – secreted in active form, hydrolysis at sn-1 and sn-3 positions, producing fatty acids and 2- monoacylglycerol - Bile salts, dietary proteins and phospholipids inhibits PTL activity - Pancreatic protein colipase enhances activity of PTL by forming complex with the PTL 3) Pancreatic alpha amylase – secreted in active form, hydrolyzes alpha- 1,4 glucose linkages but not alpha- 1,6 (Pediatric Gastrointestinal and Liver Disease, Wyllie and Hyams, 3rd edition)
- 13. Pancreatic fluid and bicarbonate secretion - Secretin- induced stimulation can increase HCO3- concentration to maximum of 140 mEq/L, creating pH of 8.2 which is necessary for action of pancreatic enzymes - Zymogen granules solubilize in alkaline medium - Pancreatic enzymes are acid sensitive - In cystic fibrosis, CFTR mutation Cl- secretion Cl-/HCO3- exchange HCO3- and Na+,K+, water in duct viscous fluid duct inspissation chronic pancreatitis
- 14. DEFINITION • Acute pancreatitis is defined as an acute inflammatory process of the pancreas with variable involvement of other regional tissues or remote organ systems • Clinical definition – at least 2 of the following 3 : (1) Abdominal pain of pancreatic origin (2) Amylase and/or lipase at least 3 times upper limits of normal (3) Imaging findings suggestive/compatible with pancreatic inflammation INSPPIRE – International Study Group of Pediatric Pancreatitis : In Search For a Cure JPGN 2018; 66: 159-76
- 15. EPIDEMIOLOGY • In children, lesser incidence than adults • Incidence vary according to the country – - USA – 13.2 cases/ 1 lac children/ year (Morinville et al., Pancreas. 2010; 39:5-8) - Australia – 3.6 cases/ 1 lac children/ year (Nydegger A et al., J Gastroenterol Hepatol. 2007; 22:1313-6) - Scarcity of data from India – Estimated 4-7 cases per year per referral centre
- 16. CLASSIFICATION • Severity in pediatric acute pancreatitis is classified as – (1) Mild – without organ failure, local or systemic complications, and usually resolves in the first week (2) Moderately severe – presence of transient organ failure that resolves in < 48 hours, or local complications or exacerbation of comorbid disease (3) Severe – persistent organ failure that lasts >48 hours and that may be involving single or multiple organs INSPPIRE – International Study Group of Pediatric Pancreatitis : In Search For a Cure
- 17. INSPPIRE – International Study Group of Pediatric Pancreatitis : In Search For a Cure
- 18. Goldstein B. et al., International Consensus Conference on Pediatrics, 2002
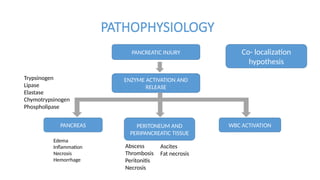
- 19. PATHOPHYSIOLOGY PANCREATIC INJURY ENZYME ACTIVATION AND RELEASE PANCREAS PERITONEUM AND PERIPANCREATIC TISSUE WBC ACTIVATION Edema Inflammation Necrosis Hemorrhage Trypsinogen Lipase Elastase Chymotrypsinogen Phospholipase Abscess Thrombosis Peritonitis Necrosis Ascites Fat necrosis Co- localization hypothesis
- 20. WBC ACTIVATION LEUKOCYTES AND MONOCYTES TISSUE DESTRUCTION LEUKOTRIENES ENDOTHELIAL AND NEUTROPHIL ACTIVATION ORGAN FAILURE Cytokines TNF- alpha PAF Proteases PMN elastase Free radicals Kidney Lung Cardiovascular shock
- 21. ETIOLOGY - Infections – Mumps, HIV, Coxsackie B, Hepatitis A,B, Varicella zoster, Measles, Leptospirosis - Biliary – Choledochal cysts, Cholelithiasis, Ascariasis, Biliary sludge - Medications – Valproate, Corticosteroids, L.Asparaginase, Azathioprine, 6- Mercaptopurine - Idiopathic – Tropical pancreatitis - Genetic – Hereditary pancreatitis, Trypsinogen gene mutation, SPINK 1 gene mutation - Structural pancreatic disorders – Annular pancreas, Pancreas divisum, Sphincter of Oddi dysfunction
- 22. - Mechanical – Blunt abdominal trauma - Metabolic – Hypertriglyceridemia, hypercalcemia - Systemic disease – Hemolytic uremic syndrome, SLE - Nutritional – Malnutrition, Vitamin A and D deficiency
- 23. ETIOLOGY • Common causes – (1) Idiopathic (52.5%) (2) Trauma (21%) (3) Biliary (10%) – Gallstones (7%), Choledochal cyst (3%) (4) Viral infections (7%) (5) Drugs (5.6%) – L-asparaginase, Valproate, Carbamazepine, Azathioprine, NSAIDS (6) Others (4%) – HUS, Macrophage activation syndrome, Post- ERCP Poddar et al., SGPGI, 2003-2014
- 24. Etiology from various studies Study Werlin et al., USA Suzuki et al., Japan Das et al., New Delhi Poddar et al., Lucknow Period/ Duration 1996-2001 1985-2011 1994-2001 2003-2014 Number of cases 180 145 28 160 Etiology (%) Idiopathic 8 8.3 35.7 52.5 Structural 19.5 39.3 10.7 10 Trauma 14 9.6 14.3 21 Drugs 12 13.1 14.3 5.6 Infectious/ viral 8 3.4 7.2 7 Systemic 14 8.9 ------- Metabolic 5.5 -------- ------- Familial 3 2.1 7.2
- 25. CLINICAL FEATURES Symptoms : More common – (1) Abdominal pain – epigastric or left upper quadrant (2) Nausea and vomiting – increases in severity in the initial 24-48h along with pain (3) Anorexia Uncommon – (4) Back pain (5) Dyspnea Das et al., AIIMS, New Delhi, 2003
- 26. Signs : More common – (1) Abdominal tenderness – mid-abdominal, generalized or epigastric tenderness (2) Low grade fever (3) Abdominal distension (4) Diminished or absent bowel sounds Uncommon – (2) Hypotension (3) Renal failure (4) Ascites (5) Pleural effusion, usually left sided (6) Fluid retention Das et al., AIIMS, New Delhi, 2003
- 27. Pancreatitis Presenter – Dr. Shefali Yadav Moderator – Dr. Raghvendra
- 28. Learning objectives • Diagnosis of acute pancreatitis • Management • Complications • Prognosis • Chronic pancreatitis – pancreatic enzymatic replacement
- 29. Diagnosis • The definition of acute pancreatitis in children is by 2 of the following: • Abdominal pain • Elevated amylase or lipase >3 times the upper limit of normal • Imaging findings of acute pancreatitis • Initial assessment – history including family history, drug intake and surgical intervention in the past, if any • Laboratory investigations – Serum amylase Serum lipase other tests
- 30. Serum amylase • α-Amylase - hydrolyzes the 1–4 glucosidic linkage in starch • Synthesized in several organs, majorly in the pancreas and salivary glands • Levels rise within hours of inflammation of the pancreas and remain increased for 1-2 days • Specificity of the serum amylase assay is highest when the increase is at least 3-fold • Serum amylase is of two categories – S-amylase and P- amylase
- 31. Serum amylase • However , 20% of adults with acute pancreatitis - normal serum amylase levels • A persistent increase - pseudocyst, pancreatic tumor or macroamylasemia • Levels don’t correlate with degree of severity of pancreatic inflammation
- 32. • Pancreatic amylase (P-amylase) Biliary obstruction Bowel obstruction Perforated duodenal ulcer Acute appendicitis Mesenteric ischemia or infarction Peritonitis Salivary amylase (S- Amylase) Salivary: parotitis (mumps), trauma, surgery, salivary duct obstruction Diabetic ketoacidosis Anorexia nervosa, bulimia Ovarian: malignancy, ruptured ectopic pregnancy, cysts Malignancy Mixed or unknown Head trauma Postoperative Macroamylasemia Causes of raised amylase
- 33. Serum lipase • Sensitivity of serum lipase is between 85% and 95% • The sensitivity of serum lipase assay is higher than that of serum amylase 24 h after the illness • As Lipase cleared by the kidney is reabsorbed by the tubules , lipase levels remain raised upto 14 days
- 34. • Other lab tests : • Complete blood count (CBC),KFT, electrolytes, albumin, glucose, and calcium • Aspartate aminotransferase (AST), alanine aminotransferase (ALT), alkaline phosphatase, gamma-glutamyl transferase (GGT), and total bilirubin • If clinical features and enzyme elevations favor pancreatitis , imaging is not required to establish the diagnosis
- 35. Conventional radiography • limited role , non specific findings • Signs seen on plain abdominal radiography – A sentinel loop - distended small bowel loop adjacent to the pancreas The colon cutoff sign - air in the splenic or hepatic flexure with a paucity of air in the distal colon Calcifications in the pancreas - chronic pancreatitis A barium study - effects of pancreatic enlargement
- 36. Sonography • Advantages - No radiation , no sedation required • Limitations – user dependent , poor image quality when air is present in the bowel overlying the pancreas
- 37. Sonography • Findings – a) diffuse or local enlargement of the pancreas b) poorly defined borders c) decreased echogenicity d) dilated pancreatic ducts e) pseudocyst f) Evaluate the gallbladder for cholelithiasis or choledocholithiasis
- 38. NORMAL PANCREAS Acute pancreatitis
- 39. Computed tomography(CECT) • Findings include diffuse enlargement of the pancreas, hemorrhage, necrosis, traumatic damage and complications such as pseudocyst • However , sedation is required • A normal CT finding does not exclude pancreatitis
- 40. Mild acute pancreatitis Necrotising pancreatitis
- 41. • Non- invasive method, no radiation and has a lower complication rate than ERCP • Diagnose structural abnormalities of the pancreaticobiliary tract and when ERCP is unsuccessful • Disadvantage -poor ability to define the peripheral biliary tree • However , an inflamed pancreas is difficult to delineate on MRCP Magnetic resonance cholangiopancreatography (MRCP)
- 43. Endoscopic retrograde cholangiopancreatography • Indications for ERCP: • Recurrent pancreatitis (more than two discrete episodes of pancreatitis) • Prolonged episode of pancreatitis (more than 1 month) • MRCP suggesting structural abnormalities • First episode of pancreatitis in a child with a family history of pancreatitis • Pancreatitis following liver transplantation • Pancreatitis associated with cystic fibrosis • Pancreatic trauma • Preoperative evaluation of non-resolving or enlarging
- 44. Endoscopic retrograde cholangiopancreatogra • Complications(in <5%) include • Pancreatitis, cholangitis • Post- procedure pain requiring analgesics • Intramural dye injection • Perforation, ileus
- 46. • Retrospective case record review of pediatric patients (age ≤15 y) undergoing ERCP between January 2011 to June 2015 • 164 ERCP procedures were done in 126 patients (67 males) • Indications : • Choledocholithiasis (50, 30.5%) • Chronic calcific pancreatitis (38,23.2%) • Main pancreatic duct injury with leak (21,12.8%) • Bile leak (12,7.3%) • The cannulation success rate was 90.4% (114 out of 126), while procedural success rate was 86% (141 out of 164) • 8(4.8%) children developed complications: • Mild pancreatitis (2) • Retroperitoneal duodenal perforation (2), • Sphincterotomyrelated bleed (2) • Hypoxia (2) Dahale, A.S., Puri, A.S., Sachdeva, S. et al. Indian Pediatr (2019) 56: 196.
- 47. Severity grading of acute pancreatitis • In adults various scoring systems are available – o Ranson criteria o Acute Physiology and Chronic Health Evaluation (APACHE)-II o Computed tomography severity index (CTSI) However, none of them are validated in pediatric population
- 48. Management Mild AP: AP without organ failure, local or systemic complications, and usually resolving within the first week Moderately severe AP : the presence of transient organ failure that resolves in no longer than 48hours, or local complications or exacerbation of co-morbid disease Severe AP : organ failure that persists for longer than 48 hours Classification of acute pancreatitis in the pediatric population: clinical report from the NASPGHAN pancre committee. Abu-El-Haija M, Kumar S, Szabo F, et al. J Pediatr Gastroenterol Nutr 2017;64:984 – 90.
- 49. • Supportive care includes careful monitoring of vital signs, ensuring bedrest and correcting intravascular fluid depletion and acidosis. • Pain management - Intravenous morphine or other opioid should be used for acute pancreatitis pain not responding to acetaminophen or NSAIDs • Look for complications • Mild disease - The treatment is mainly supportive and includes intravenous fluid resuscitation and pain management • Severe pancreatitis- address local, systemic and septic complications while providing supportive care OVERVIEW OF MANAGEMENT
- 50. Fluid resuscitation in AP Purpose of effective fluid resuscitation - replenish the blood volume, stabilize the capillary permeability, modulate the inflammatory reaction, and sustain intestinal barrier function Colloids and/or crystalloids: Among crystalloids, lactate Ringer’s better than normal saline. Use colloids especially when albumin < 2.0 g/dL or hematocrit < 35% A “controlled” resuscitation aimed at reversing hypotension, and being able to maintain effective mean arterial pressure (MAP) and urine output > 0.5 mL/kg/hr Aggarwal A, Manrai M, Kochhar R. Fluid resuscitation in acute pancreatitis. World J Gastroenterol. 2014;20(48):18092–18103
- 51. Children with diagnosis of acute pancreatitis should be provided 1.5–2x maintenance IV fluids with monitoring of urine output over the next 24–48h Based on assessment of hydration status/hemodynamic status, if evidence of hemodynamic compromise, a bolus of 10–20mL/kg is recommended The IAP/APA guidelines recommend that patients receive 5–10 ml/kg/hr until resuscitation goals are achieved with regards to improvements in heart rate, urine output, mean arterial pressure and/or hematocrit Abu-El-Haija M, Kumar S, Quiros JA, et al. Management of Acute Pancreatitis in the Pediatric Population: A Clinical Report From the North American Society for Pediatric Gastroenterology, Hepatology and Nutrition Pancreas Committee. J Pediatr Gastroenterol Nutr. 2018;66(1):159–176
- 52. Monitoring • Vitals should be strictly monitored to decide both the rate of hydration as well as the early detection of complications, if any : Cardiovascular Monitoring - HR, Bp, urine output Pulmonary Monitoring - ABG (PaO2), CXR Renal Monitoring – KFT, Urine ouput
- 53. Nutrition During Acute Pancreatitis Enteral Nutrition (Oral, Gastric, Jejunal) During an Episode of Acute Pancreatitis Enteral Versus Parenteral Nutrition in Acute Pancreatitis Timing of Initiation of Enteral Feedings in Acute Pancreatitis Gastric Versus Jejunal Feeding in Acute Pancreatitis Diet/Formula Composition in Acute Pancreatitis “Nutritional Considerations in Pediatric Pancreatitis: A Position Paper from the NASPGHAN Pancreas Committ ESPGHAN Cystic Fibrosis/Pancreas Working Group.” Abu-El-Haija, Maisam et al. Journal of pediatric gastroenterology and nutrition vol. 67,1 (2018): 131-143.
- 54. • Mild AP • Should be started on a general (regular) diet and advanced as tolerated • Should be nourished preferably via mouth as compared to nasogastric route • EN(enteral nutrition) is favored over PN(parenteral nutrition) when possible • Jejunal tube feedings should be reserved for those unable to tolerate oral or nasogastric tube • Parenteral mode of nutrition should be used when oral/ NG/NJ feeds are not tolerated • Combination of EN and PN, rather than PN alone, should be used in children who do not meet caloric goals with EN alone “Nutritional Considerations in Pediatric Pancreatitis: A Position Paper from the NASPGHAN Pancreas Committee and ESPGHAN Cystic Fibrosis/Pancreas Working Group.” Abu-El-Haija, Maisam et al. Journal of pediatric gastroenterology and nutrition vol. 67,1 (2018): 131-143.
- 55. • Severe AP • Enteral nutrition (oral, NG or NJ as tolerated) should be attempted in children with SAP within 72 hours from presentation to medical care, once deemed hemodynamically stable • Jejunal tube feeding should be reserved for those unable to tolerate oral or NG tube feeding • The use of specialized formulas or immunonutrition is not necessary “Nutritional Considerations in Pediatric Pancreatitis: A Position Paper from the NASPGHAN Pancreas Committee and ESPGHAN Cystic Fibrosis/Pancreas Working Group.” Abu-El-Haija, Maisam et al. Journal of pediatric gastroenterology and nutrition vol. 67,1 (2018): 131-143.
- 56. Complications of pancreatitis • Local complications : Pseudo cyst- • localized collection in the lesser sac • Clinical features - vomiting, pain abdomen, mass palpable per abdomen • Imaging – Usg, ct will help define the problem • Complications include – hemorrhage, infection or rupture • Management - <4cm usually resolve spontaneously, some may drain on its own into stomach or colon, others require intervention – endoscopic or surgical
- 57. Complications of pancreatitis • Other local complications : Abscess Necrosis
- 58. Systemic Complications of pancreatitis Respiratory Pleural effusion Adult respiratory distress syndrome Cardiovascular Shock Fluid loss/ sequestration Bleeding Pericarditis Myocardial depression Renal failure Hypovolemia Shock DIC Central nervous system Psychosis or coma Dermatologic Fat necrosis Hematologic Disseminated intravascular coagulation Hemolysis Thrombocytopenia Metabolic Hypocalcemia Acidosis Hyperlipidemia Hyperkalemia Gastrointestinal Paralytic ileus Hemorrhage Stress ulcers Colonic obstruction/ fistula/ wall erosion Splenic hematoma/ rupture
- 59. Recurrent pancreatitis • Definition : ≥ 2 discrete episodes of AP , failure to meet AP criteria for a period after first episode and absence of evidence of irreversible structural changes in pancreas • Pancreatitis-associated gene mutations are the most common risk factors - PRSS1 ,SPINK1 • PERT should not be routinely used in children diagnosed with ARP, who do not have exocrine pancreatic insufficiency
- 60. • From January 2003 to December 2015, 93 consecutive children (≤18 years of age) diagnosed to have ARP were included in this study • A baseline Magnetic resonance cholangiopancreatography (MRCP) done in all cases • Serum calcium, lipid profile, blood sugar and stool fat (Sudan stain) were done in all cases • Genetic markers (PRSS1, SPINK1, and CFTR) were studied in a group of 22 idiopathic ARP casesdiagnosed to have ARP were included in this study • Etiology wise – MC- IDIOPATHIC, f/b biliopancreatic structural causes • ARP, especially in those with idiopathic and genetic mutations, is a precursor of chronic pancreatitis(CP) and acts as a transition phase between AP and CP Poddar, Ujjal & Yachha, Surender & Borkar, Vibhor & Srivastava, Anshu. (2017). Is acute recurrent pancreatitis in children a precursor of chronic pancreatitis? A long-term follow-up study of 93 cases. Digestive and Liver Disease. 49. 10.1016/j.dld.2017.02.019.
- 62. Pathophysiology • Continuous destruction of the pancreatic gland resulting in irreversible scarring of the acinar and ductal cells • About 90% of the gland must be destroyed before clinical signs of pancreatic dysfunction occur • There is infiltration of the glandular tissue by lym- phocytes, plasma cells and macrophages • Each flare results in further damage and eventually leads to exocrine and endocrine dysfunction • Pancreatic ducts show fibrosis, stricture and dilation. Calcification within the gland may be seen
- 63. Causes Obstructive ● Congenital ductal anomalies- Pancreas divisum Choledochal cyst Stricture ● Trauma ● Sclerosing cholangitis ● Idiopathic fibrosing cholangitis ● Autoimmune pancreatitis ● Secondary to other autoimmune disorders Calcific • Hereditary causes: • PRSS1 SPINK1 CFTR mutations ?Mesotrypsin mutation ?Anionic trypsin mutation ● Tropical pancreatitis ● Hyperlipidemia ● Hypercalcemia ● Organic acidemias Miscellaneous ● Idiopathic ● Mitochondrial cytopathy ● Inflammatory bowel disease
- 64. Clinical features Chronic abdominal pain with episodic exacerbation Eventually pain improves- burning out of pancreas- exocrine and endocrine pancreatic insufficiency Exocrine insufficiency - hyperphagia to compensate for the gastrointestinal malabsorptive losses ,secondary growth failure, stools – malodorous and features of protein and fat malabsorption Endocrine insufficiency – adulthood diabetes(3c) Children with chronic pancreatitis should be screened for pancreatic exocrine insufficiency every 6 to 12 months
- 65. • Children <19 years of age were considered eligible for inclusion in the study if they met criteria for ARP and/or CP • Those patients who had total pancreatectomy (TP) with or without islet autotransplantation (IAT)-were excluded • 6% of children diagnosed with DM • 40% of children in the registry with a diagnosis of DM having a diagnosis of CP and 60%, having ARP • 5 children with DM also had beta cell antibodies(38%) • DM was more common in those children who also had hypertriglyceridemia and other autoimmune disorders • Thus,a multitude of risk factors were present and not just pancreatitis Bellin MD et al. Diabetes Mellitus in Children with Acute Recurrent and Chronic Pancreatitis: Data From the INternational Study Group of Pediatric Pancreatitis: In Search for a CuRE Cohort. J Pediatr Gastroenterol Nutr. 2019 Nov;69(5) 599-606.
- 66. Diagnosis • Serum amylase and lipase are raised – eventually decrease once pancreatic destruction occurs • Calcifications in the pancreas on CT or plain radiography • ERCP/MRCP- beading of ducts (narrowing and dilation) • Genetic testing – PRSS1, SPINK 1, CTRC,CFTR
- 68. Diagnosis • Fecal elastase-1 (FE-1)on formed stool - used for the diagnosis of Exocrine Pancreatic Insufficiency - a value less than 100 μg/g is diagnostic • 72-h fecal fat test - coefficient of fat absorption [CFA: (grams of fat ingested-grams of fat excreted)/(grams of fat ingested) x100] can be calculated - absorption value of <85% of fat intake is considered abnormal in children younger than 6 months of age, and < 93% is abnormal for children older than 6 months of age • Direct pancreatic secretion testing (collection of pancreatic/intestinal fluid) is considered invasive and not commonly used
- 69. Management • Exacerbations – treated like acute pancreatitis • PAIN – multimodal treatment Non-medication therapies - distraction, visual imaging Integrative pain strategies such as aromatherapy, acupuncture Non-opioid medications Opioids Hospitalization with inpatient pain management
- 70. PAIN MANAGEMENT • No specific pediatric guidelines exist • Medical therapies include acetaminophen, nonsteroidal anti-inflammatory drugs and narcotic analgesics • Non-narcotic analgesics should be the first line of therapy for pain, and narcotics reserved for uncontrollable pain • Surgical therapies - drainage procedures to decompress obstructed ducts, resection of strictures and removal of pancreatic stones . • Total pancreatectomy and islet auto transplantation may be indicated in children with CP and intractable pain, unresponsive to other measures Párniczky, Andrea & Abu-El-Haija, Maisam & Husain, Sohail & Lowe, Mark & Oracz, Grzegorz & Sahin-Tóth, Miklós & Szabo, Flora & Uc, Aliye & Wilschanski, Michael & Witt, Heiko & Czakó, László & Grammatikopoulos, Tassos & Rasmussen, Ib & Sutton, Robert & Hegyi, Peter. (2018). EPC/HPSG evidence-based guidelines for the management of pediatric pancreatitis. Pancreatology. 18. 10.1016/j.pan.2018.01.001.
- 71. Total pancreatectomy and islet auto transplantation • INDICATIONS : 1.Pain or debilitation for >6 months, as demonstrated by one of the following: a. Chronic opioid dependence for >6 months b. Severely impaired quality of life (frequent school absence and/or hospitalizations) 2. Failure of maximal medical and endoscopic therapies 3. Absence of reversible cause of CP or ARP 4. Absence of physiologic or psychosocial contraindication 5. Willingness to accept risk of lifelong diabetes 6. Adequate islet function (absence of C-peptide negative diabetes) Párniczky, Andrea & Abu-El-Haija, Maisam & Husain, Sohail & Lowe, Mark & Oracz, Grzegorz & Sahin-Tóth, Miklós & Szabo, Flora & Uc, Aliye & Wilschanski, Michael & Witt, Heiko & Czakó, László & Grammatikopoulos, Tassos & Rasmussen, Ib & Sutton, Robert & Hegyi, Peter. (2018). EPC/HPSG evidence-based guidelines for the management of pediatric pancreatitis. Pancreatology. 18. 10.1016/j.pan.2018.01.001.
- 72. Dosing of PERT • Not known for children with Chronic pancreatitis • However doses well defined for children with Cystic Fibrosis- 1000 to 2500 lipase units/kg per meal in < 4 years of age and 500–2500 lipase units/kg per meal are used for those > 4 years of age • Lipase may also be based on grams of fat ingested : 500–4000 units lipase per gram fat . For snacks, half the dose is recommended • Infants - 2,000 to 4,000 units per 120 mL of infant formula or per breast- feeding. • Doses are adjusted based on effect (clinical, stool, growth) “Nutritional Considerations in Pediatric Pancreatitis: A Position Paper from the NASPGHAN Pancreas Committee and ESPGHAN Cystic Fibrosis/Pancreas Working Group.” Abu-El-Haija, Maisam et al. Journal of pediatric gastroenterology and nutrition vol. 67,1 (2018): 131-143.
- 73. DRUG COMPANY CONTENTS PRICE(INR) Creon Solvay Lipase-10000 IU, amylase – 8000 IU, protease – 600 IU 205.5 Leno - EZ Bestochem Alpha galactosidase A 200mg, lactase 7mg, protease 25mg , amylase 50mg,lipase 3mg 57 Digemax Shreya Lipase 20000 u, amylase 62250 u, protease 93750 u 145 Pan lipase Sun Lipase 10000 USP u, protease 37000 USP u, amylase 33200 USP u 120.80
- 76. FOLLOW UP • Growth and nutritional status • Fat soluble vitamin levels – vit D, PT-INR • Development of exocrine and endocrine pancreatic insufficiency • Psychosocial assessment – missed school days, pain control
- 77. Ministry of Health, Labour and Welfare of Japan (JPN) scoring 1. Base excess ≤ -3 mEq or shock (systolic blood pressure cutoffs according to age group); 2. PaO2 ≤ 60 mmHg (room air) or respiratory failure; 3. Blood urea nitrogen ≥ 40 mg/dL [or creatinine (Cr) ≥ 2.0 mg/dL] or oliguria (< 0.5 mL/kg per h); 4. Lactate dehydrogenase ≥ 2 × the value of the upper limits; 5. Platelet count ≤ 1 × 105 /mm3 ; 6. Calcium ≤ 7.5 mg/dL; 7. C-reactive protein ≥ 15 mg/dL; 8. Number of positive measures in pediatric SIRS score ≥ 3; 9. Age < 7 years old or/and weight < 23 kg • The cutoff for predicting a severe outcome was set at three criteria • Sensitivity - 80% & specificity - 96% Suzuki, Mitsuyoshi et al. “Scoring system for the prediction of severe acute pancreatitis in children.” Pediatrics international : official journal of the Japan Pediatric Society 57 1 (2015): 113-8
- 78. CT SEVERITY INDEX (CTSI) • Grading of pancreatitis (Balthazar score) • A: normal pancreas: 0 • B: enlargement of pancreas: 1 • C: inflammatory changes in pancreas and peripancreatic fat: 2 • D: ill-defined single peripancreatic fluid collection: 3 • E: two or more poorly defined peripancreatic fluid collections: 4 • Pancreatic necrosis • none: 0 • ≤30%: 2 • >30-50%: 4 • >50%: 6 • Scoring : 0-3: mild acute pancreatitis • 4-6: moderate acute pancreatitis • 7-10: severe acute pancreatitis
Editor's Notes
- #34: Elevations in these tests suggest concomitant liver disease and/or bile duct obstruction.
- #36: Presence of pancreatitis Cause of pancreatitis like biliary stones Complicationa like pseudocyst
- #38: A- normal pancreas, b- bulky pancreas
- #39: CONTRAST UPTAKE ENHANCED IN INFLAMMATION, DECREASED UPTAKE- NECROSIS Grading of pancreatitis (Balthazar score) A: normal pancreas: 0 B: enlargement of pancreas: 1 C: inflammatory changes in pancreas and peripancreatic fat: 2 D: ill-defined single peripancreatic fluid collection: 3 E: two or more poorly defined peripancreatic fluid collections: 4 Pancreatic necrosis none: 0 ≤30%: 2 >30-50%: 4 >50%: 6 Scoring : 0-3: mild acute pancreatitis 4-6: moderate acute pancreatitis 7-10: severe acute pancreatitis
- #40: PIC 1- BULKY PANCREAS , NORMAL ENHANCING PIC2- PANCREAS WITH AREAS OF NON ENHANCEMENT(ARROW) AND AREAS OF NORMAL ENHANCEMENT (STAR)- NECROTISING PACREATITIS
- #41: Not usually orderd – only structural causes or gallstone pancreatitis with inconsistenrt findings Secretin is sometimes administered during the procedure to stimulate pancreatic fluid secretion, resulting in dilation of the pancreatic ducts and enhancing their visualization [21,22,28]. The value of the secretin test in children is somewhat controversial. Secretin-stimulated MRCP may also provide indirect evidence of pancreatic exocrine function based on the volume of fluid in the proximal intestine after secretin stimulation
- #42: 2 image – pancreatic divisum
- #60: SGPGI LUCKNOW STUDY Mri - todetect structural causes ofARP andalso to rule outthepresence of chronic pancreatitis (CP). Patients were followed up every 3–6 monthly. If symptoms persisted (episodes of pancreatitis) a repeat MRCP was done after 1–2 years to look for the changes of chronic pancreatitis. A Biliopancreatic- choledochal cyst, divisum, diverticulum and gall stones
- #64: type 3c diabetes [19]. The primary abnormality is decreased insulin secretion, similar to type 1 diabetes. However, pancreatic diabetes is also characterized by impaired secretion of glucagon, which leads to hypoglycemia due to loss of the pancreatic counterregulatory mechanism.
- #65: One of the primary mechanisms leading to the development of pancreatogenic DM is bystander destruction of the islets (and beta cells) as pancreatic parenchyma is replaced by fibrosis in CP. . In addition to a trend towards increased odds for other autoimmune disorders, 5 of 13 tested were positive for beta cell autoimmunity (38%) n increased prevalence of beta cell autoimmunity in patients with cystic fibrosis (CF) who develop CF-related diabetes (CFRD), a different form of pancreatogenic diabetes. Onset of CFRD occurred at a younger age in patients with beta cell autoantibodies (
- #66: serine protease 1 gene (PRSS1) that encodes cationic trypsinogen in up to 80 percent of families with hereditary pancreatitis. SPINK1 – There is a weaker association between chronic pancreatitis and mutations in the serine protease inhibitor Kazal type 1 gene (SPINK1). SPINK1 mutations probably act as disease modifiers, lowering the threshold for pancreatitis caused by other genetic or environmental factors CTRC – Chymotrypsin C (CTRC) is an enzyme that protects the pancreas by eliminating prematurely activated trypsin.
- #67: 1- usg showing calcifications 2- ercp showing dilated pancreatic ductwith blunting of side branches, dilated cbd with stenosis of distal bile duct opening
- #68: The test should not be performed during an episode of acute pancreatitis because results may be temporarily low. Similarly, the test should not be performed in a patient with diarrhea because results will be falsely low levels due to dilution.
- #72: Activates feedback control of pancreatic secretion by reducing realease of CCK and destroying CCK releasing factor.
- #73: U is the amount of enzyme that converts one micro mole of substrate per min IU is under standard conditions
- #74: Cost 7000-8000
- #76: Exocrine- fecal elastase- measures human elastase and not pert-porcine


































































![Diagnosis
• Fecal elastase-1 (FE-1)on formed stool - used for the diagnosis of Exocrine Pancreatic
Insufficiency - a value less than 100 μg/g is diagnostic
• 72-h fecal fat test - coefficient of fat absorption [CFA: (grams of fat ingested-grams of fat
excreted)/(grams of fat ingested) x100] can be calculated - absorption value of <85% of fat intake
is considered abnormal in children younger than 6 months of age, and < 93% is abnormal for
children older than 6 months of age
• Direct pancreatic secretion testing (collection of pancreatic/intestinal fluid) is considered invasive
and not commonly used](https://image.slidesharecdn.com/acutepancreatitiscombined-250827030659-7d322359/85/ACUTE-PANCREATITIS-combined-pptx-pptx-in-kids-68-320.jpg)







![Ministry of Health, Labour and Welfare of
Japan (JPN) scoring
1. Base excess ≤ -3 mEq or shock (systolic blood pressure cutoffs according to age group);
2. PaO2 ≤ 60 mmHg (room air) or respiratory failure;
3. Blood urea nitrogen ≥ 40 mg/dL [or creatinine (Cr) ≥ 2.0 mg/dL] or oliguria (< 0.5 mL/kg per h);
4. Lactate dehydrogenase ≥ 2 × the value of the upper limits;
5. Platelet count ≤ 1 × 105
/mm3
;
6. Calcium ≤ 7.5 mg/dL;
7. C-reactive protein ≥ 15 mg/dL;
8. Number of positive measures in pediatric SIRS score ≥ 3;
9. Age < 7 years old or/and weight < 23 kg
• The cutoff for predicting a severe outcome was set at three criteria
• Sensitivity - 80% & specificity - 96%
Suzuki, Mitsuyoshi et al. “Scoring system for the prediction of severe acute pancreatitis
in children.” Pediatrics international : official journal of the Japan Pediatric Society 57 1
(2015): 113-8](https://image.slidesharecdn.com/acutepancreatitiscombined-250827030659-7d322359/85/ACUTE-PANCREATITIS-combined-pptx-pptx-in-kids-77-320.jpg)
