Genetic testing of breast and ovarian cancer patients: clinical characteristics and hormonal risk modifiers
- 1. European Journal of Obstetrics & Gynecology and Reproductive Biology 85 (1999) 75–80 Genetic testing of breast and ovarian cancer patients: clinical characteristics and hormonal risk modifiers a a a b a b Luna Kaduri , Maya Gibs , Ayala Hubert , Michal Sagi , Norman Heching , Israela Lerer , a b b a , *Bietrice Uziely , Naomi Weinberg , Dvorah Abeliovich , Tamar Peretz a Sharett Institute of Oncology, Hadassah Hebrew University Hospital, Ein Kerem, P.O. Box 12000, Jerusalem, Israel 91120 b Department Human Genetics, Hadassah Hebrew University Hospital, Jerusalem, Israel Abstract Objectives: Carriers of the mutations 185delAG and 5382insC in the BRCA1 gene and 6174delT in the BRCA2 gene have a substantial life-time risk for breast and ovarian cancers (BC and OC). The aim of the study was to identify the clinical features and the hormonal risk modifiers in mutation carriers and the implication in suggested guidelines for treatment decisions in BRCA1/2 carrier patients. Study design: Breast and/or ovarian cancer patients from the Oncology and Cancer Genetic clinics were tested for the three Ashkenazi founder mutations: 87 patients were identified as carriers of one of these mutations. Clinical presentation and age at onset were correlated with the mutations, in patients with bilateral BC or BC and OC, the length of time that elapsed between the diagnosis of the two cancers was recorded. We compared BC and OC patients with regard to ages at menarche, first pregnancy and menopause, number of pregnancies and deliveries, the use of oral contraceptives, hormonal replacement therapy and fertility treatments. Results: The carriers of the three BRCA1/2 Ashkenazi founder mutations did not differ in clinical presentation nor age at onset. Forty-three patients (74.1%) of 58 BC patients were diagnosed between the ages 30 and 50, only four (6.9%) patients were diagnosed after age 60. Of BC patients diagnosed before age 35, 63.6% developed second BC as compared to 25.5% of those diagnosed after age 35. Ovarian cancer was diagnosed after age 45 in 89.7% of the patients, only one patient was diagnosed under the age of 40. Oral contraceptives use was documented in 61.3% of BC patients as compared to 11.8% of OC patients. Other hormonal factors did not differ between the two groups. Conclusions: The carriers of the three Ashkenazi founder mutations should be considered at the same risk for BC and for OC and treatment options should be the same. Mutation carriers diagnosed with BC before the age of 35 are at a very high risk for developing second breast cancer. Most ovarian cancers in carriers were diagnosed after age 45, and prophylactic oophorectomy should be postponed to the age of 45. Oral contraceptives might elevate the risk of BC in mutation carriers. © 1999 Elsevier Science Ireland Ltd. All rights reserved. Keywords: Breast cancer; Ovarian cancer; BRCA1/2; Ashkenazi founder mutations; Hormonal effects; Prevention 1. Introduction for ovarian cancer (OC) [5,6]. Carriers that were ascer- tained from the general population (not necessarily with a The identification of the BRCA1 and BRCA2 genes positive family history for BC/OC), were estimated to have led to population based studies. Three founder have a life-time risk of 30–56% for BC and 6–16% for mutations, 185delAG [1] and 5382insC [2] in the BRCA1 ovarian cancer [7,8]. The difference in the risk of develop- gene and the mutation 6174delT [3] in the BRCA2 gene, ing BC/OC in these two groups of carriers suggests that were reported in the Jewish Ashkenazi population (Jews different genetic and environmental factors and life style, who originated in central Europe). These mutations have a might interact with BRCA1 and BRCA2 genes and modify combined frequency of approximately 2.6% in this popula- the risk in mutation carriers. Two studies investigated the tion [4]. correlation between hormonal factors and clinical diag- The life-time risk in carriers from high-risk families was nosis in BRCA1/2 carriers. The risk for BC in BRCA1 estimated to be 70–85% for breast cancer (BC) and 50% carriers was found to decline with increasing parity, in the same way as in the general population, whereas a first * pregnancy at a young age did not confer additionalCorresponding author. Tel.: 1972-2-6777825; fax: 1972-2-6427485. E-mail address: tamarp@cc.huji.ac.il (T. Peretz) protection [9]. A study conducted in Ashkenazi BC 0301-2115/99/$ – see front matter © 1999 Elsevier Science Ireland Ltd. All rights reserved. PII: S0301-2115(98)00286-3
- 2. 76 L. Kaduri et al. / European Journal of Obstetrics & Gynecology and Reproductive Biology 85 (1999) 75–80 patients diagnosed at a young age suggested that the use of 2.2. Mutation analysis oral contraceptives might increase the risk of BC in BRCA1/2 carriers then in non-carriers [10]. Multiplex PCR was performed for the three Ashkenazi To date, the preventative means offered to individuals at founder mutations, 185delAG, 5382insC (BRCA1) and high-risk for BC or OC are surveillance, prophylactic 6174delT (BRCA2) as previously described [14]. surgeries, and chemoprevention. Screening mammography in the general population decreases the relative risk of 2.3. Statistical analysis mortality by 30% [11]. The efficacy of mammography for women younger than 40 years is low. Other modes of Age at onset according to different mutations was screening using ultrasound and MRI are under inves- compared using the ANOVA test for continuous variables. tigation. Screening for ovarian cancer has not been proven The effect of hormonal factors was compared between to reduce mortality [12,13]. breast and ovarian cancer patients using ANOVA test for 2 The present study was conducted among Jewish BC/OC continuous variables and the x test for discrete variables. patients, carriers of one of the three BRCA1/2 Ashkenazi founder mutations. The aim of the study was to present the clinical characteristics of these patients regarding the 3. Results clinical presentation and age at onset in the different mutation carriers. In addition we evaluated the correlation Among the BC and OC patients examined for the between several hormonal factors and clinical presentation mutations 185delAG, 5382insC or 6174delT, 87 were in carriers. The implications of our conclusions are dis- found to carry one of the three mutation, most of them cussed in suggested guidelines for treatment decisions. were from high-risk families. Forty-two (48.3%) were carriers of the mutation 185delAG, thirty-seven (42.5%) carried the 6174delT mutation and seven (8.0%) were 2. Patients and methods carriers of the mutation 5382insC. One patient with OC was a double heterozygote, a carrier of two BRCA 2.1. Patients mutations, 185delAG in BRCA1 and 6174delT in BRCA2 [15]. Since clinically she did not differ from the rest of the Blood samples were collected from patients with BC group, arbitrarily she was included in the 6174delT group. and/or OC. The patients were referred either from the Oncology clinic or from the Cancer-Genetic Counseling 3.1. Clinical presentation of carriers clinic. Some of the patients were from high-risk families (with a positive family history for BC/OC in at least three The patients were classified according to their clinical first-degree relatives), the rest were sporadic cases, some of presentation (Table 1). Among the carriers of the the carriers were previously described [14]. All patients 185delAG mutation (n542), 27 (64.3%) were diagnosed signed an informed consent approved by the Ethical with BC (with or without ovarian cancer afterwards) as Committee. Eighty-seven patients were identified as car- compared to 24/38 (63.2%) of carriers of the 6174delT riers of a BRCA1/2 mutation, they were the focus of our mutation. OC was diagnosed in 21/42 (50%) carriers of study. Eighty-four of the carrier patients were of Ashken- the 185delAG mutation and in 19/38 (50%) carriers of the azi origin, two of the carriers of the 185delAG mutation 6174delT mutation. The number of 5382insC carriers was were of Iraqi origin, and one came from North Africa. small, all of them developed BC only. Reproductive and hormonal histories of the patients The mean age of BC and OC diagnosis in the carrier were obtained from the examinee and were confirmed in patients according to the mutation is presented in Table 2. the medical files. The clinical presentation and mutations In all patients who had both BC and OC, BC was the first in the patients are presented in Table 1. to appear. The mean age at diagnosis of BC was 43.6 and 47.0 in carriers of the mutations 185delAG and 6174delT, Table 1 Clinical presentation in carrier patients according to mutation type Table 2 Age at diagnosis according to mutation type Diagnosis No. of carriers Diagnosis 185delAG 6174delT 5382insC 185delAG 6174delT 5382insC Total a d Breast cancer 43.6612 47.0610.8 39.867.5 N.S. Breast cancer 12 13 5 30 b c Ovarian cancer 52.168 58.5613 N.S. Bilateral breast cancer 9 6 2 17 a Breast and ovarian cancer 5 4 0 9 All breast cancer patients including those diagnosed with ovarian cancer Bilateral breast cancer 1 1 0 2 afterwards. b Ovarian cancer 15 14 0 29 All ovarian cancer patients including those that had breast cancer. c Age at diagnosis of one patient was unknown. Total 42 38 7 87 d Not significant in ANOVA test.
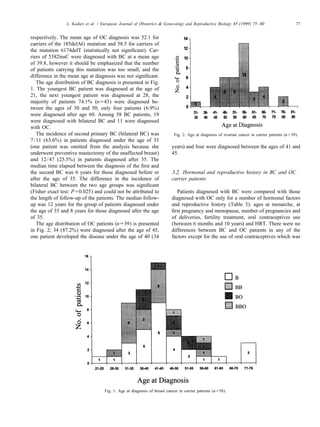
- 3. L. Kaduri et al. / European Journal of Obstetrics & Gynecology and Reproductive Biology 85 (1999) 75–80 77 respectively. The mean age of OC diagnosis was 52.1 for carriers of the 185delAG mutation and 58.5 for carriers of the mutation 6174delT (statistically not significant). Car- riers of 5382insC were diagnosed with BC at a mean age of 39.8, however it should be emphasized that the number of patients carrying this mutation was too small, and the difference in the mean age at diagnosis was not significant. The age distribution of BC diagnosis is presented in Fig. 1. The youngest BC patient was diagnosed at the age of 21, the next youngest patient was diagnosed at 28, the majority of patients 74.1% (n543) were diagnosed be- tween the ages of 30 and 50, only four patients (6.9%) were diagnosed after age 60. Among 58 BC patients, 19 were diagnosed with bilateral BC and 11 were diagnosed with OC. The incidence of second primary BC (bilateral BC) was Fig. 2. Age at diagnosis of ovarian cancer in carrier patients (n539). 7/11 (63.6%) in patients diagnosed under the age of 35 (one patient was omitted from the analysis because she years) and four were diagnosed between the ages of 41 and underwent preventive mastectomy of the unaffected breast) 45. and 12/47 (25.5%) in patients diagnosed after 35. The median time elapsed between the diagnosis of the first and the second BC was 6 years for those diagnosed before or 3.2. Hormonal and reproductive history in BC and OC after the age of 35. The difference in the incidence of carrier patients bilateral BC between the two age groups was significant (Fisher exact test: P50.025) and could not be attributed to Patients diagnosed with BC were compared with those the length of follow-up of the patients. The median follow- diagnosed with OC only for a number of hormonal factors up was 12 years for the group of patients diagnosed under and reproductive history (Table 3): ages at menarche, at the age of 35 and 8 years for those diagnosed after the age first pregnancy and menopause, number of pregnancies and of 35. of deliveries, fertility treatment, oral contraceptives use The age distribution of OC patients (n539) is presented (between 6 months and 10 years) and HRT. There were no in Fig. 2; 34 (87.2%) were diagnosed after the age of 45, differences between BC and OC patients in any of the one patient developed the disease under the age of 40 (34 factors except for the use of oral contraceptives which was Fig. 1. Age at diagnosis of breast cancer in carrier patients (n558).
- 4. 78 L. Kaduri et al. / European Journal of Obstetrics & Gynecology and Reproductive Biology 85 (1999) 75–80 Table 3 Hormonal and obstetric characteristics of the BRCA carrier patients Characteristic Patients Breast cancer Ovarian cancer a Age at menarche 13.261.3 12.761.3 N.S. a Age at first pregnancy 25.464.7 24.163.5 N.S. a No. of pregnancies 3.561.9 4.562.9 N.S. a No. of deliveries 2.461.4 2.461.4 N.S. a Age at menopause 46.865.2 47.864.7 N.S. b Use of oral contraceptives 61.3% 11.8% ,0.01 c Fertility treatments 13.8% 13.3% N.S. c Hormonal replacement therapy 11.8% 33.0% N.S. a Not significant in ANOVA test. b 2 P in x test. c 2 Not significant in x test. 61.3% among BC patients as compared to 11.8% in OC category for bilateral BC. Therefore, a carrier patient who only patients (P,0.01). was diagnosed with BC under the age of 35 could be protected from second BC by bilateral mastectomy. Scharg et al. [16] and Grann et al. [17] showed a 2.8–5.3 year 4. Discussion gain for bilateral mastectomy done at the age of 30 in a healthy carrier. The year gain for high-risk patients was The availability of genetic testing and the awareness of higher than for carriers at a lower risk according to the the general population of genetic predisposition to cancer family history. A carrier patient that has already been made genetic testing widespread, especially for BC and diagnosed with BC, is at risk of mortality and the year gain OC families. However, little is known about the sur- provided by prophylactic mastectomy of the unaffected veillance and treatment that should be recommended to breast might be lower than that for a healthy carrier. Yet, patients who were identified as carriers. the subgroup of carrier patients diagnosed under the age of The purpose of this study was to identify specific risk 35 is at-high risk for another BC, and the survival gained factors in carriers of the BRCA1/2 mutations and to by the procedure might overcome the decreased survival suggest guidelines for treatment and appropriate follow-up by the first primary BC. Patients’ acceptance of prophylac- for these patients. tic surgeries is low [18] and most decisions regarding The incidence of BC and OC was the same among the prophylactic mastectomy are undertaken while the patient carriers of the 185delAG and 6174delT mutations. The has already been diagnosed with breast cancer. We suggest seven carriers of the 5382insC mutation had BC only, but using the age at BC diagnosis as a guideline in offering subsequent patients in our clinic, who were identified as prophylactic mastectomy. BC carriers who were diagnosed carriers of the 5382insC mutation were diagnosed with after the age of 35 could be offered a breast conservation OC. Thus, the number of 5382insC carriers was too small surgery. Robson et al. [19] reported an ipsilateral recur- to evaluate phenotype–genotype correlation. rence rate of 12% in 5 years after breast conservation The mean age at diagnosis of BC was 10 years younger therapy in carriers of a BRCA1/2 mutation, they did not than that of OC in all the carriers. There was a tendency relate to age at diagnosis. Interestingly, the rate of con- towards a higher age at presentation in carriers of the tralateral BC in the same group of patients was higher, and 6174delT mutation as compared to carriers of the 185delT this might suggest that irradiation of the breast protected it mutation, but statistically the difference was not signifi- from a second primary BC, thus bilateral irradiation could cant. Therefore, carriers of the mutations 185delAG and be another option in these patients. This issue should be 6174delT should be considered at the same risk for BC and pursued further in a larger number of patients. for OC and the treatment options should be the same. The age distribution of OC diagnosis in our group of Age at diagnosis of BC divided the patients into two patients could be used as a guideline for preferred age for distinct subgroups, regardless of the mutation they carry. prophylactic oophorectomy. All but one OC patient were Patients diagnosed with BC at a young age (,35) had a diagnosed at the age of 40 or older, most of them were higher probability of having second BC (63.6%) as diagnosed between the ages of 46 and 60. Two studies compared to those diagnosed at the age 35 or older [16,17] suggest a gain of 0.5–2 years for bilateral (25.5%). The median time between the diagnosis of the oophorectomy if performed at age 30, but delayed first and the second BC was the same for both groups. This oophorectomy of 10 years, for a 30-year-old woman, did observation suggests that other factors, genetic or en- not cause loss of life expectancy, our data support this vironmental put the young group of patients in a high-risk conclusion. Treatment could also be tailored according to
- 5. L. Kaduri et al. / European Journal of Obstetrics & Gynecology and Reproductive Biology 85 (1999) 75–80 79 the mutation found in each patient. The age at diagnosis of the risk of BC in carriers more than in non-carriers. OC seems to be higher in carriers of the 6174delAT Prospective studies on the role of oral contraceptives in mutation than in carriers of the 185delAG mutation. Only modifying cancer risk in BRCA1/2 carriers, are warranted. one out of the nineteen OC patients carrying the 6174delT Narod et al. [9] found higher OC risk for carriers born mutation was diagnosed at the age of 41, the rest were before 1930 regardless of oral contraceptive use. It could diagnosed at the age of 45 or older, thus bilateral be that various unknown factors are responsible for this oophorectomy in 6174delAG carriers, could be postponed difference, and the difference in our OC and BC patients, to age 45. The timing of prophylactic surgeries is im- was attributed to the same factors. portant for the patients’ quality of life. Oophorectomy at a Based on our experience we suggest that oral contracep- younger age can cause impaired body image and sexual tives should not be offered to carriers as a prevention dysfunction. It causes early menopause and the patient means for OC since it might elevate the risk of BC. For should be treated with long-term HRT. Although we do young carriers the use of low dose estrogen pills as not yet have data regarding the risk conferred by HRT in contraceptives should not be denied, no data exists regard- BRCA1/2 carriers, it is reasonable to postpone the pro- ing the cancer risk that is conferred by these pills, even in cedure as long as possible. Patients’ acceptance of the general population. The safety of HRT in carriers is prophylactic oophorectomy would probably be higher if also unknown. We have not found any difference between suggested close to the physiologic menopause. To date, we BC and OC patients with regard to HRT, but many of the recommend bilateral oophorectomy at the age of 45 to all patients that were studied by us, were diagnosed at the mutation carriers. However, carriers of the 185delAG premenoupausal age, and the number of patients who used mutation might be at risk at a younger age, therefore the HRT was low in the study groups. We do not recommend option of earlier prophylactic surgeries should be discussed HRT after prophylactic oophorectomy unless the patients with these carriers. suffer from the symptoms of menopause, for these patients The influence of different hormonal factors in the we recommend short-term HRT. Other menopause-related BRCA1/2 carriers was analyzed in the BC patients and risks such as coronary heart disease and osteoporosis OC only patients. Since the average age at diagnosis of BC should be considered in each case. preceded the average age at diagnosis of OC by 10 years, To conclude, treatment decision in BRCA1/2 carriers is we hypothesized that the group of OC only patients, might difficult for both patients and their doctors and even more be protected from BC and survived to the age of onset of complex in healthy carriers. Our study provides guidelines OC. In the general population exposure to estrogens is based on clinical features and hormonal risk modifiers that known to elevate the risk for BC [20]. Therefore, early were retrospectively analyzed in a group of carrier patients. menarche and late menopause are risk factors for BC. Oral This data should serve us until we have a prospective contraceptives and HRT might elevate the risk as well. randomized trials. The data should be presented to each Early menarche and late menopause also elevate the risk of patient and the treatment options should be discussed in developing OC, whereas multiple pregnancies and oral the decision making process. contraceptive use reduce the risk [20]. In a study on human BC cell lines [21], the expression of BRCA1 mRNA increased upon stimulation with estrogen and progesterone. References It could be that steroids stimulate proliferation and in- directly increase BRCA1 mRNA and protein. In the same [1] Simard J, Tonin P, Durocher F, Morgan K, Rommens J, Gingras S, way, germ-line mutations in BRCA1/2 may affect cellular Samson C, et al. Common origin of BRCA1 mutations in Canadian breast and ovarian cancer families. Nat Genet 1994;8:392–8.response to hormonal stimuli. [2] Berman DB, Wagner-Costalas J, Schultz DC, Lynch HT, Daly M,None of the hormonal factors mentioned above were Godwin AK. Two distinct origins of a common BRCA1 mutation in found to be significantly different between BC and OC breast-ovarian cancer families: a genetic study of 15 185delAG patients except for oral contraceptive use which might mutation kindreds. Am J Hum Genet 1996;58:1166–76. elevate the risk of BC carriers. This conclusion should be [3] Neuhausen SL, Gilewski T, Norton L, Tram T, McGuire P, Swensen considered carefully, since the age structure of the two J, Hampel H, et al. Recurrent BRCA2 6174delT mutation in Ashkenazi Jewish women affected by breast cancer. Nat Genetgroups, of the BC and of the OC patients, was different. 1996;13:126–8. The BC patients were younger, therefore they had higher [4] Fodor FH, Weston A, Bleiweiss IJ, McCurdy LD, et al. Frequency exposure to oral contraceptives. In addition the number of and carrier risk associated with common BRCA1 and BRCA2 patients was too small to subset analyses. Ursin et al. [10] mutations in Ashkenazi Jewish breast cancer patients. Am J Hum reached the same conclusion using as a control group Genet 1998;63:45–51. [5] Claus EB, Schildkraut JM, Thompson WP, Risch NJ. The geneticnon-carrier Ashkenazi BC patients of the same age and attributable risk of breast and ovarian cancer. Cancer 1996;77:2318– from the same socioeconomic and cultural background. In 24. this study [10], the use of oral contraceptives before the [6] Miki Y, Swensen J, Shuttuck ED, et al. A strong candidate for the first pregnancy was higher among carriers than non-car- breast and ovarian susceptibility gene BRCA1. Science riers, suggesting that oral contraceptive use may increase 1994;266:66–71.
- 6. 80 L. Kaduri et al. / European Journal of Obstetrics & Gynecology and Reproductive Biology 85 (1999) 75–80 [7] Struewing JP, Hartge P, Wacholder S, et al. The risk of cancer breast cancer patients among Ashkenazi woman. Am J Hum Genet associated with specific mutations of BRCA1 and BRCA2 among 1997;60:505–14. Ashkenazi Jews. New Engl J Med 1997;336:1401–8. [15] Friedman E, Bar-Sade Bruchim R, Kruglikova A. Double [8] Whittemore AS, Gong G, Itngre J. Prevalence and contribution of heterozygotes for the Ashkenazi founder mutations in BRCA1 and BRCA1 mutations in breast cancer and ovarian cancer: results from BRCA2 genes. Am J Hum Genet 1998;63:1224–7. three US population-based case–control studies of ovarian cancer. [16] Schrag D, Kunts KM, Garber JE, Weeks JC. Decision analysis-effect Am J Hum Genet 1997;60:496–504. of prophylactic mastectomy and oophorectomy on life expectancy [9] Narod SA, Goldgar D, Canon-Albright L, Weber B, Moslehi R, Ives among women with BRCA1 or BRCA2 mutations. New Engl J Med E, Lenoir G, Lynch H. Risk modifiers in carriers of BRCA1 1997;336:1465–71. mutations. Int J Can 1995;64:394–8. [17] Grann VR, Panageas KS, Whang W, Antman KH, Neugut AI. [10] Ursin G, Henderson BE, Haile RW, Pike MC, Zhou N, Diep A, Decision analysis of prophylactic mastectomy and oophorectomy in Bernstein L. Does oral contraceptive use increase the risk of breast BRCA1 positive or BRCA2 positive patients. J Clin Oncol cancer in women with BRCA1/BRCA2 mutations more than in 1998;16:979–85. other women. Cancer Res 1997;57:3678–81. [18] Eisinger F, Renoire JC, Chabal F, Loquet C, Moatti J, Sobol H. [11] Fletcer SW, Black W, Harris R, Rimer BK, Shapiro S. Report of the Acceptable strategies for dealing with hereditary breast/ovarian international workshop on screening for breast cancer. J Natl Cancer cancer risk. J Natl Cancer Inst 1997;89:731. Inst 1993;85(20):1644–56. [19] Robson M, Levine D, Brown B, et al. Results of breast conservation [12] Jacobs I, Bridges J, Reynolds C, et al. Multimodal approach to therapy for invasive breast cancer in women with BRCA mutations. screening for ovarian cancer. Lancet 1988;2:268–71. Proc Am Soc Clin Oncol 1998;17:2103. [13] Einhorn N, Sjovall K, Schoenfeld DA, et al. Prospective evaluation [20] Henderson BE, Ross RK, Pike MC. Hormonal chemoprevention in of the specificity of serum CA125 levels for detection of ovarian women. Science 1993;259:633–8. cancer in normal population. Am Soc Clin Oncol 1990;9:157. [21] Gudas JM, Ngugen H, Li T, Cowan KH. Hormone dependant [14] Abeliovich D, Kaduri L, Lerer I, Weinberg N, et al. The founder regulation of BRCA1 in human breast cancer cells. Cancer Res mutations 185delAG and 5382insc in BRCA1 and 6174delT in 1995;55:4561–5. BRCA2 appear in 60% of ovarian cancer and 30% of early onset

![European Journal of Obstetrics & Gynecology
and Reproductive Biology 85 (1999) 75–80
Genetic testing of breast and ovarian cancer patients: clinical
characteristics and hormonal risk modifiers
a a a b a b
Luna Kaduri , Maya Gibs , Ayala Hubert , Michal Sagi , Norman Heching , Israela Lerer ,
a b b a ,
*Bietrice Uziely , Naomi Weinberg , Dvorah Abeliovich , Tamar Peretz
a
Sharett Institute of Oncology, Hadassah Hebrew University Hospital, Ein Kerem, P.O. Box 12000, Jerusalem, Israel 91120
b
Department Human Genetics, Hadassah Hebrew University Hospital, Jerusalem, Israel
Abstract
Objectives: Carriers of the mutations 185delAG and 5382insC in the BRCA1 gene and 6174delT in the BRCA2 gene have a substantial
life-time risk for breast and ovarian cancers (BC and OC). The aim of the study was to identify the clinical features and the hormonal risk
modifiers in mutation carriers and the implication in suggested guidelines for treatment decisions in BRCA1/2 carrier patients. Study
design: Breast and/or ovarian cancer patients from the Oncology and Cancer Genetic clinics were tested for the three Ashkenazi founder
mutations: 87 patients were identified as carriers of one of these mutations. Clinical presentation and age at onset were correlated with the
mutations, in patients with bilateral BC or BC and OC, the length of time that elapsed between the diagnosis of the two cancers was
recorded. We compared BC and OC patients with regard to ages at menarche, first pregnancy and menopause, number of pregnancies and
deliveries, the use of oral contraceptives, hormonal replacement therapy and fertility treatments. Results: The carriers of the three
BRCA1/2 Ashkenazi founder mutations did not differ in clinical presentation nor age at onset. Forty-three patients (74.1%) of 58 BC
patients were diagnosed between the ages 30 and 50, only four (6.9%) patients were diagnosed after age 60. Of BC patients diagnosed
before age 35, 63.6% developed second BC as compared to 25.5% of those diagnosed after age 35. Ovarian cancer was diagnosed after
age 45 in 89.7% of the patients, only one patient was diagnosed under the age of 40. Oral contraceptives use was documented in 61.3% of
BC patients as compared to 11.8% of OC patients. Other hormonal factors did not differ between the two groups. Conclusions: The
carriers of the three Ashkenazi founder mutations should be considered at the same risk for BC and for OC and treatment options should
be the same. Mutation carriers diagnosed with BC before the age of 35 are at a very high risk for developing second breast cancer. Most
ovarian cancers in carriers were diagnosed after age 45, and prophylactic oophorectomy should be postponed to the age of 45. Oral
contraceptives might elevate the risk of BC in mutation carriers. © 1999 Elsevier Science Ireland Ltd. All rights reserved.
Keywords: Breast cancer; Ovarian cancer; BRCA1/2; Ashkenazi founder mutations; Hormonal effects; Prevention
1. Introduction for ovarian cancer (OC) [5,6]. Carriers that were ascer-
tained from the general population (not necessarily with a
The identification of the BRCA1 and BRCA2 genes positive family history for BC/OC), were estimated to
have led to population based studies. Three founder have a life-time risk of 30–56% for BC and 6–16% for
mutations, 185delAG [1] and 5382insC [2] in the BRCA1 ovarian cancer [7,8]. The difference in the risk of develop-
gene and the mutation 6174delT [3] in the BRCA2 gene, ing BC/OC in these two groups of carriers suggests that
were reported in the Jewish Ashkenazi population (Jews different genetic and environmental factors and life style,
who originated in central Europe). These mutations have a might interact with BRCA1 and BRCA2 genes and modify
combined frequency of approximately 2.6% in this popula- the risk in mutation carriers. Two studies investigated the
tion [4]. correlation between hormonal factors and clinical diag-
The life-time risk in carriers from high-risk families was nosis in BRCA1/2 carriers. The risk for BC in BRCA1
estimated to be 70–85% for breast cancer (BC) and 50% carriers was found to decline with increasing parity, in the
same way as in the general population, whereas a first
* pregnancy at a young age did not confer additionalCorresponding author. Tel.: 1972-2-6777825; fax: 1972-2-6427485.
E-mail address: tamarp@cc.huji.ac.il (T. Peretz) protection [9]. A study conducted in Ashkenazi BC
0301-2115/99/$ – see front matter © 1999 Elsevier Science Ireland Ltd. All rights reserved.
PII: S0301-2115(98)00286-3](https://image.slidesharecdn.com/genetictestingofbreastandovarianca-160328035746/85/Genetic-testing-of-breast-and-ovarian-cancer-patients-clinical-characteristics-and-hormonal-risk-modifiers-1-320.jpg)
![76 L. Kaduri et al. / European Journal of Obstetrics & Gynecology and Reproductive Biology 85 (1999) 75–80
patients diagnosed at a young age suggested that the use of 2.2. Mutation analysis
oral contraceptives might increase the risk of BC in
BRCA1/2 carriers then in non-carriers [10]. Multiplex PCR was performed for the three Ashkenazi
To date, the preventative means offered to individuals at founder mutations, 185delAG, 5382insC (BRCA1) and
high-risk for BC or OC are surveillance, prophylactic 6174delT (BRCA2) as previously described [14].
surgeries, and chemoprevention. Screening mammography
in the general population decreases the relative risk of 2.3. Statistical analysis
mortality by 30% [11]. The efficacy of mammography for
women younger than 40 years is low. Other modes of Age at onset according to different mutations was
screening using ultrasound and MRI are under inves- compared using the ANOVA test for continuous variables.
tigation. Screening for ovarian cancer has not been proven The effect of hormonal factors was compared between
to reduce mortality [12,13]. breast and ovarian cancer patients using ANOVA test for
2
The present study was conducted among Jewish BC/OC continuous variables and the x test for discrete variables.
patients, carriers of one of the three BRCA1/2 Ashkenazi
founder mutations. The aim of the study was to present the
clinical characteristics of these patients regarding the 3. Results
clinical presentation and age at onset in the different
mutation carriers. In addition we evaluated the correlation Among the BC and OC patients examined for the
between several hormonal factors and clinical presentation mutations 185delAG, 5382insC or 6174delT, 87 were
in carriers. The implications of our conclusions are dis- found to carry one of the three mutation, most of them
cussed in suggested guidelines for treatment decisions. were from high-risk families. Forty-two (48.3%) were
carriers of the mutation 185delAG, thirty-seven (42.5%)
carried the 6174delT mutation and seven (8.0%) were
2. Patients and methods carriers of the mutation 5382insC. One patient with OC
was a double heterozygote, a carrier of two BRCA
2.1. Patients mutations, 185delAG in BRCA1 and 6174delT in BRCA2
[15]. Since clinically she did not differ from the rest of the
Blood samples were collected from patients with BC group, arbitrarily she was included in the 6174delT group.
and/or OC. The patients were referred either from the
Oncology clinic or from the Cancer-Genetic Counseling 3.1. Clinical presentation of carriers
clinic. Some of the patients were from high-risk families
(with a positive family history for BC/OC in at least three The patients were classified according to their clinical
first-degree relatives), the rest were sporadic cases, some of presentation (Table 1). Among the carriers of the
the carriers were previously described [14]. All patients 185delAG mutation (n542), 27 (64.3%) were diagnosed
signed an informed consent approved by the Ethical with BC (with or without ovarian cancer afterwards) as
Committee. Eighty-seven patients were identified as car- compared to 24/38 (63.2%) of carriers of the 6174delT
riers of a BRCA1/2 mutation, they were the focus of our mutation. OC was diagnosed in 21/42 (50%) carriers of
study. Eighty-four of the carrier patients were of Ashken- the 185delAG mutation and in 19/38 (50%) carriers of the
azi origin, two of the carriers of the 185delAG mutation 6174delT mutation. The number of 5382insC carriers was
were of Iraqi origin, and one came from North Africa. small, all of them developed BC only.
Reproductive and hormonal histories of the patients The mean age of BC and OC diagnosis in the carrier
were obtained from the examinee and were confirmed in patients according to the mutation is presented in Table 2.
the medical files. The clinical presentation and mutations In all patients who had both BC and OC, BC was the first
in the patients are presented in Table 1. to appear. The mean age at diagnosis of BC was 43.6 and
47.0 in carriers of the mutations 185delAG and 6174delT,
Table 1
Clinical presentation in carrier patients according to mutation type Table 2
Age at diagnosis according to mutation type
Diagnosis No. of carriers
Diagnosis 185delAG 6174delT 5382insC
185delAG 6174delT 5382insC Total
a d
Breast cancer 43.6612 47.0610.8 39.867.5 N.S.
Breast cancer 12 13 5 30 b c
Ovarian cancer 52.168 58.5613 N.S.
Bilateral breast cancer 9 6 2 17
a
Breast and ovarian cancer 5 4 0 9 All breast cancer patients including those diagnosed with ovarian cancer
Bilateral breast cancer 1 1 0 2 afterwards.
b
Ovarian cancer 15 14 0 29 All ovarian cancer patients including those that had breast cancer.
c
Age at diagnosis of one patient was unknown.
Total 42 38 7 87 d
Not significant in ANOVA test.](https://image.slidesharecdn.com/genetictestingofbreastandovarianca-160328035746/85/Genetic-testing-of-breast-and-ovarian-cancer-patients-clinical-characteristics-and-hormonal-risk-modifiers-2-320.jpg)
![78 L. Kaduri et al. / European Journal of Obstetrics & Gynecology and Reproductive Biology 85 (1999) 75–80
Table 3
Hormonal and obstetric characteristics of the BRCA carrier patients
Characteristic Patients
Breast cancer Ovarian cancer
a
Age at menarche 13.261.3 12.761.3 N.S.
a
Age at first pregnancy 25.464.7 24.163.5 N.S.
a
No. of pregnancies 3.561.9 4.562.9 N.S.
a
No. of deliveries 2.461.4 2.461.4 N.S.
a
Age at menopause 46.865.2 47.864.7 N.S.
b
Use of oral contraceptives 61.3% 11.8% ,0.01
c
Fertility treatments 13.8% 13.3% N.S.
c
Hormonal replacement therapy 11.8% 33.0% N.S.
a
Not significant in ANOVA test.
b 2
P in x test.
c 2
Not significant in x test.
61.3% among BC patients as compared to 11.8% in OC category for bilateral BC. Therefore, a carrier patient who
only patients (P,0.01). was diagnosed with BC under the age of 35 could be
protected from second BC by bilateral mastectomy. Scharg
et al. [16] and Grann et al. [17] showed a 2.8–5.3 year
4. Discussion gain for bilateral mastectomy done at the age of 30 in a
healthy carrier. The year gain for high-risk patients was
The availability of genetic testing and the awareness of higher than for carriers at a lower risk according to the
the general population of genetic predisposition to cancer family history. A carrier patient that has already been
made genetic testing widespread, especially for BC and diagnosed with BC, is at risk of mortality and the year gain
OC families. However, little is known about the sur- provided by prophylactic mastectomy of the unaffected
veillance and treatment that should be recommended to breast might be lower than that for a healthy carrier. Yet,
patients who were identified as carriers. the subgroup of carrier patients diagnosed under the age of
The purpose of this study was to identify specific risk 35 is at-high risk for another BC, and the survival gained
factors in carriers of the BRCA1/2 mutations and to by the procedure might overcome the decreased survival
suggest guidelines for treatment and appropriate follow-up by the first primary BC. Patients’ acceptance of prophylac-
for these patients. tic surgeries is low [18] and most decisions regarding
The incidence of BC and OC was the same among the prophylactic mastectomy are undertaken while the patient
carriers of the 185delAG and 6174delT mutations. The has already been diagnosed with breast cancer. We suggest
seven carriers of the 5382insC mutation had BC only, but using the age at BC diagnosis as a guideline in offering
subsequent patients in our clinic, who were identified as prophylactic mastectomy. BC carriers who were diagnosed
carriers of the 5382insC mutation were diagnosed with after the age of 35 could be offered a breast conservation
OC. Thus, the number of 5382insC carriers was too small surgery. Robson et al. [19] reported an ipsilateral recur-
to evaluate phenotype–genotype correlation. rence rate of 12% in 5 years after breast conservation
The mean age at diagnosis of BC was 10 years younger therapy in carriers of a BRCA1/2 mutation, they did not
than that of OC in all the carriers. There was a tendency relate to age at diagnosis. Interestingly, the rate of con-
towards a higher age at presentation in carriers of the tralateral BC in the same group of patients was higher, and
6174delT mutation as compared to carriers of the 185delT this might suggest that irradiation of the breast protected it
mutation, but statistically the difference was not signifi- from a second primary BC, thus bilateral irradiation could
cant. Therefore, carriers of the mutations 185delAG and be another option in these patients. This issue should be
6174delT should be considered at the same risk for BC and pursued further in a larger number of patients.
for OC and the treatment options should be the same. The age distribution of OC diagnosis in our group of
Age at diagnosis of BC divided the patients into two patients could be used as a guideline for preferred age for
distinct subgroups, regardless of the mutation they carry. prophylactic oophorectomy. All but one OC patient were
Patients diagnosed with BC at a young age (,35) had a diagnosed at the age of 40 or older, most of them were
higher probability of having second BC (63.6%) as diagnosed between the ages of 46 and 60. Two studies
compared to those diagnosed at the age 35 or older [16,17] suggest a gain of 0.5–2 years for bilateral
(25.5%). The median time between the diagnosis of the oophorectomy if performed at age 30, but delayed
first and the second BC was the same for both groups. This oophorectomy of 10 years, for a 30-year-old woman, did
observation suggests that other factors, genetic or en- not cause loss of life expectancy, our data support this
vironmental put the young group of patients in a high-risk conclusion. Treatment could also be tailored according to](https://image.slidesharecdn.com/genetictestingofbreastandovarianca-160328035746/85/Genetic-testing-of-breast-and-ovarian-cancer-patients-clinical-characteristics-and-hormonal-risk-modifiers-4-320.jpg)
![L. Kaduri et al. / European Journal of Obstetrics & Gynecology and Reproductive Biology 85 (1999) 75–80 79
the mutation found in each patient. The age at diagnosis of the risk of BC in carriers more than in non-carriers.
OC seems to be higher in carriers of the 6174delAT Prospective studies on the role of oral contraceptives in
mutation than in carriers of the 185delAG mutation. Only modifying cancer risk in BRCA1/2 carriers, are warranted.
one out of the nineteen OC patients carrying the 6174delT Narod et al. [9] found higher OC risk for carriers born
mutation was diagnosed at the age of 41, the rest were before 1930 regardless of oral contraceptive use. It could
diagnosed at the age of 45 or older, thus bilateral be that various unknown factors are responsible for this
oophorectomy in 6174delAG carriers, could be postponed difference, and the difference in our OC and BC patients,
to age 45. The timing of prophylactic surgeries is im- was attributed to the same factors.
portant for the patients’ quality of life. Oophorectomy at a Based on our experience we suggest that oral contracep-
younger age can cause impaired body image and sexual tives should not be offered to carriers as a prevention
dysfunction. It causes early menopause and the patient means for OC since it might elevate the risk of BC. For
should be treated with long-term HRT. Although we do young carriers the use of low dose estrogen pills as
not yet have data regarding the risk conferred by HRT in contraceptives should not be denied, no data exists regard-
BRCA1/2 carriers, it is reasonable to postpone the pro- ing the cancer risk that is conferred by these pills, even in
cedure as long as possible. Patients’ acceptance of the general population. The safety of HRT in carriers is
prophylactic oophorectomy would probably be higher if also unknown. We have not found any difference between
suggested close to the physiologic menopause. To date, we BC and OC patients with regard to HRT, but many of the
recommend bilateral oophorectomy at the age of 45 to all patients that were studied by us, were diagnosed at
the mutation carriers. However, carriers of the 185delAG premenoupausal age, and the number of patients who used
mutation might be at risk at a younger age, therefore the HRT was low in the study groups. We do not recommend
option of earlier prophylactic surgeries should be discussed HRT after prophylactic oophorectomy unless the patients
with these carriers. suffer from the symptoms of menopause, for these patients
The influence of different hormonal factors in the we recommend short-term HRT. Other menopause-related
BRCA1/2 carriers was analyzed in the BC patients and risks such as coronary heart disease and osteoporosis
OC only patients. Since the average age at diagnosis of BC should be considered in each case.
preceded the average age at diagnosis of OC by 10 years, To conclude, treatment decision in BRCA1/2 carriers is
we hypothesized that the group of OC only patients, might difficult for both patients and their doctors and even more
be protected from BC and survived to the age of onset of complex in healthy carriers. Our study provides guidelines
OC. In the general population exposure to estrogens is based on clinical features and hormonal risk modifiers that
known to elevate the risk for BC [20]. Therefore, early were retrospectively analyzed in a group of carrier patients.
menarche and late menopause are risk factors for BC. Oral This data should serve us until we have a prospective
contraceptives and HRT might elevate the risk as well. randomized trials. The data should be presented to each
Early menarche and late menopause also elevate the risk of patient and the treatment options should be discussed in
developing OC, whereas multiple pregnancies and oral the decision making process.
contraceptive use reduce the risk [20]. In a study on human
BC cell lines [21], the expression of BRCA1 mRNA
increased upon stimulation with estrogen and progesterone. References
It could be that steroids stimulate proliferation and in-
directly increase BRCA1 mRNA and protein. In the same [1] Simard J, Tonin P, Durocher F, Morgan K, Rommens J, Gingras S,
way, germ-line mutations in BRCA1/2 may affect cellular Samson C, et al. Common origin of BRCA1 mutations in Canadian
breast and ovarian cancer families. Nat Genet 1994;8:392–8.response to hormonal stimuli.
[2] Berman DB, Wagner-Costalas J, Schultz DC, Lynch HT, Daly M,None of the hormonal factors mentioned above were
Godwin AK. Two distinct origins of a common BRCA1 mutation in
found to be significantly different between BC and OC
breast-ovarian cancer families: a genetic study of 15 185delAG
patients except for oral contraceptive use which might mutation kindreds. Am J Hum Genet 1996;58:1166–76.
elevate the risk of BC carriers. This conclusion should be [3] Neuhausen SL, Gilewski T, Norton L, Tram T, McGuire P, Swensen
considered carefully, since the age structure of the two J, Hampel H, et al. Recurrent BRCA2 6174delT mutation in
Ashkenazi Jewish women affected by breast cancer. Nat Genetgroups, of the BC and of the OC patients, was different.
1996;13:126–8.
The BC patients were younger, therefore they had higher
[4] Fodor FH, Weston A, Bleiweiss IJ, McCurdy LD, et al. Frequency
exposure to oral contraceptives. In addition the number of and carrier risk associated with common BRCA1 and BRCA2
patients was too small to subset analyses. Ursin et al. [10] mutations in Ashkenazi Jewish breast cancer patients. Am J Hum
reached the same conclusion using as a control group Genet 1998;63:45–51.
[5] Claus EB, Schildkraut JM, Thompson WP, Risch NJ. The geneticnon-carrier Ashkenazi BC patients of the same age and
attributable risk of breast and ovarian cancer. Cancer 1996;77:2318–
from the same socioeconomic and cultural background. In
24.
this study [10], the use of oral contraceptives before the [6] Miki Y, Swensen J, Shuttuck ED, et al. A strong candidate for the
first pregnancy was higher among carriers than non-car- breast and ovarian susceptibility gene BRCA1. Science
riers, suggesting that oral contraceptive use may increase 1994;266:66–71.](https://image.slidesharecdn.com/genetictestingofbreastandovarianca-160328035746/85/Genetic-testing-of-breast-and-ovarian-cancer-patients-clinical-characteristics-and-hormonal-risk-modifiers-5-320.jpg)
![80 L. Kaduri et al. / European Journal of Obstetrics & Gynecology and Reproductive Biology 85 (1999) 75–80
[7] Struewing JP, Hartge P, Wacholder S, et al. The risk of cancer breast cancer patients among Ashkenazi woman. Am J Hum Genet
associated with specific mutations of BRCA1 and BRCA2 among 1997;60:505–14.
Ashkenazi Jews. New Engl J Med 1997;336:1401–8. [15] Friedman E, Bar-Sade Bruchim R, Kruglikova A. Double
[8] Whittemore AS, Gong G, Itngre J. Prevalence and contribution of heterozygotes for the Ashkenazi founder mutations in BRCA1 and
BRCA1 mutations in breast cancer and ovarian cancer: results from BRCA2 genes. Am J Hum Genet 1998;63:1224–7.
three US population-based case–control studies of ovarian cancer. [16] Schrag D, Kunts KM, Garber JE, Weeks JC. Decision analysis-effect
Am J Hum Genet 1997;60:496–504. of prophylactic mastectomy and oophorectomy on life expectancy
[9] Narod SA, Goldgar D, Canon-Albright L, Weber B, Moslehi R, Ives among women with BRCA1 or BRCA2 mutations. New Engl J Med
E, Lenoir G, Lynch H. Risk modifiers in carriers of BRCA1 1997;336:1465–71.
mutations. Int J Can 1995;64:394–8. [17] Grann VR, Panageas KS, Whang W, Antman KH, Neugut AI.
[10] Ursin G, Henderson BE, Haile RW, Pike MC, Zhou N, Diep A, Decision analysis of prophylactic mastectomy and oophorectomy in
Bernstein L. Does oral contraceptive use increase the risk of breast BRCA1 positive or BRCA2 positive patients. J Clin Oncol
cancer in women with BRCA1/BRCA2 mutations more than in 1998;16:979–85.
other women. Cancer Res 1997;57:3678–81. [18] Eisinger F, Renoire JC, Chabal F, Loquet C, Moatti J, Sobol H.
[11] Fletcer SW, Black W, Harris R, Rimer BK, Shapiro S. Report of the Acceptable strategies for dealing with hereditary breast/ovarian
international workshop on screening for breast cancer. J Natl Cancer cancer risk. J Natl Cancer Inst 1997;89:731.
Inst 1993;85(20):1644–56. [19] Robson M, Levine D, Brown B, et al. Results of breast conservation
[12] Jacobs I, Bridges J, Reynolds C, et al. Multimodal approach to therapy for invasive breast cancer in women with BRCA mutations.
screening for ovarian cancer. Lancet 1988;2:268–71. Proc Am Soc Clin Oncol 1998;17:2103.
[13] Einhorn N, Sjovall K, Schoenfeld DA, et al. Prospective evaluation [20] Henderson BE, Ross RK, Pike MC. Hormonal chemoprevention in
of the specificity of serum CA125 levels for detection of ovarian women. Science 1993;259:633–8.
cancer in normal population. Am Soc Clin Oncol 1990;9:157. [21] Gudas JM, Ngugen H, Li T, Cowan KH. Hormone dependant
[14] Abeliovich D, Kaduri L, Lerer I, Weinberg N, et al. The founder regulation of BRCA1 in human breast cancer cells. Cancer Res
mutations 185delAG and 5382insc in BRCA1 and 6174delT in 1995;55:4561–5.
BRCA2 appear in 60% of ovarian cancer and 30% of early onset](https://image.slidesharecdn.com/genetictestingofbreastandovarianca-160328035746/85/Genetic-testing-of-breast-and-ovarian-cancer-patients-clinical-characteristics-and-hormonal-risk-modifiers-6-320.jpg)